- Safety & Recalls
- Regulatory Updates
- Drug Coverage
- COPD
- Cardiovascular
- Obstetrics-Gynecology & Women's Health
- Ophthalmology
- Clinical Pharmacology
- Pediatrics
- Urology
- Pharmacy
- Idiopathic Pulmonary Fibrosis
- Diabetes and Endocrinology
- Allergy, Immunology, and ENT
- Musculoskeletal/Rheumatology
- Respiratory
- Psychiatry and Behavioral Health
- Dermatology
- Oncology
Aliskiren: A novel oral renin inhibitor for the treatment of hypertension
Cardiac function is regulated in part by the renin-angiotensin-aldosterone system, and current cardiovascular therapies work to antagonize this system by inhibiting the generation or action of angiotensin II. Aliskiren is the first drug to be reviewed by FDA in a new class of antihypertensive agents that directly inhibit the action of renin.
Abstract
Cardiac function is regulated in part by the renin-angiotensin-aldosterone system, and current cardiovascular therapies work to antagonize this system by inhibiting the generation or action of angiotensin II. Aliskiren is the first drug to be reviewed by FDA in a new class of antihypertensive agents that directly inhibit the action of renin, the rate-limiting step in the system, thus theoretically antagonizing the renin-angiotensin-aldosterone system to a greater extent than current treatments. Aliskiren achieves superior blood pressure reduction compared with placebo and has a blood pressure-lowering effect similar to or better than that of hydrochlorothiazide, ramipril, irbesartan, and losartan. Aliskiren is well tolerated, with nonspecific adverse events occurring at a rate similar to that seen with placebo and other comparators and hyperkalemia occurring with a frequency similar to that observed with an angiotensin-converting enzyme inhibitor. Aliskiren rarely causes hypotension when used in combination therapies. An NDA for aliskiren was submitted to FDA in April 2006. If approved, aliskiren will be a new option for the management of hypertension. Additional studies will be needed to determine if there is a role for this agent in other disease states, including heart failure, coronary artery disease, and nephropathy. (Formulary. 2006;41:631–638.)
The renin-angiotensin-aldosterone system (RAAS) is a major regulator of cardiac function. The central role of the RAAS is exemplified by the importance of agents that antagonize this system (angiotensin-converting enzyme [ACE] inhibitors, angiotensin receptor blockers [ARBs], and aldosterone antagonists) in the management of cardiovascular diseases. Aldosterone antagonism, inhibition of the formation of angiotensin II with an ACE inhibitor, or inhibition of the action of angiotensin II at the angiotensin II type I (AT1) receptor with an ARB results in significant reduction in morbidity and mortality among patients with hypertension, heart failure, coronary artery disease, and nephropathy.1,2
Release of renin is the rate-limiting step in the RAAS. Renin is released from the kidneys and converts angiotensinogen to angiotensin.1 As such, renin is responsible for all "downstream" events leading to production of angiotensin II and stimulation of the AT1 and AT2 receptors. Therefore, a medication that inhibits renin could theoretically antagonize the RAAS to a greater extent than an agent that antagonizes the generation or action of angiotensin II. Aliskiren (Novartis) is the first agent under review in this new class of renin inhibitors. The manufacturer submitted an NDA for aliskiren to FDA in April 2006.
CHEMISTRY AND PHARMACOLOGY
Aliskiren binds with high affinity to the catalytic portion of human renin.4 This agent is a highly specific inhibitor of renin and has little to no effect on other human enzymes.4 Aliskiren also has no effect on adrenergic, serotonergic, histamine, opiate, benzodiazepine, or adenosine receptors.4
To determine the effect of agents such as aliskiren on renin concentration, researchers can measure renin through 2 methods. The first method, which analyzes plasma renin activity (PRA), measures the enzymatic activity of renin and quantifies the amount of angiotensin I generated from renin activity.5 The high-affinity binding of aliskiren to renin leads to a rapid reduction in PRA.6 This inhibition of PRA appears to persist for approximately 3 to 6 hours with low doses (40–80 mg/d) and 10 to 48 hours with higher doses (160–640 mg/d) of aliskiren.6,7 PRA is reduced dose dependently, with the greatest reductions occurring when the highest doses are used.5 Upon withdrawal of aliskiren, PRA does not return to pretreatment levels for approximately 2 weeks.8 Conversely, both ACE inhibitors and ARBs have been observed to increase PRA to a greater extent than placebo. This increase occurs a few hours after the ACE inhibitor or ARB is administered, and PRA remains elevated throughout therapy.5–7 When aliskiren is added to an ARB or ACE inhibitor, PRA is lower than with the ARB or ACE inhibitor alone and higher than with aliskiren monotherapy.6,9,10
The other method for quantifying renin is the measurement of plasma active renin, also known as active renin concentration (ARC). Measurement of ARC allows for quantification of the amount of renin present, regardless of whether it is active.6 ARC is elevated early after treatment with aliskiren and remains elevated with repeated dosing.7 As with PRA, ARC does not return to pretreatment levels until 2 weeks after withdrawal.8 Elevation in ARC is greater with aliskiren than with the ARB valsartan.6 ARC likely is increased because the amounts of both angiotensin I and angiotensin II are reduced by aliskiren for at least 24 hours after treatment administration.6 A feedback loop signaling the kidneys to release more renin is triggered by low levels of angiotensin II; therefore, an increase in ARC is a marker of RAAS suppression.1 The higher ARC observed with aliskiren compared with that observed with ACE inhibitors or ARBs suggests that aliskiren provides more complete suppression of the RAAS. Although ARBs inhibit the action of angiotensin II at the AT1 receptor and ACE inhibitors prevent the generation of angiotensin II, ARBs also increase both angiotensin I and II, whereas ACE inhibitors increase angiotensin I.6,7 Increased angiotensin I could lead to increased generation of angiotensin II by alternative pathways, and more angiotensin II could lead to increased stimulation of AT2 receptors, which are not blocked by ARBs. ARC may be higher with aliskiren because this agent inhibits the RAAS at a point before these alternative pathways or sites of action and targets the only known pathway for conversion of angiotensinogen to angiotensin I.
Finally, animal data suggest that aliskiren also has a significant effect on cardiac and renal damage associated with hypertension. In a rat model, the degree of albuminuria with the administration of low-dose (0.3 mg/kg/d) or high-dose (3 mg/kg/d) aliskiren for 8 weeks was less than with no treatment or with low doses of the ARB valsartan (1 mg/kg/d) and similar to that seen with high-dose valsartan (10 mg/kg/d).11 In the same study, cardiac hypertrophy was reduced with both low- and high-dose aliskiren, and high-dose valsartan plus high-dose aliskiren reduced cardiac hypertrophy to a greater extent than high-dose valsartan alone.11
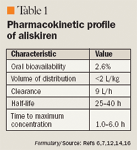
PHARMACOKINETICS
CLINICAL TRIALS
The overwhelming majority of the clinical data regarding aliskiren involve studies of patients with hypertension. In these studies, aliskiren has been compared with both placebo and commonly used antihypertensive agents (Table 2). The majority of hypertension trials with aliskiren have been conducted in patients with mild-to-moderate hypertension. It should be noted that most of the clinical trials with aliskiren are available in abstract form only; only 2 of the studies have been published as full manuscripts.5,17
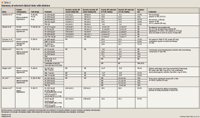
Hypertension: comparative/combination trials. Aliskiren also has been compared to or combined with other antihypertensive agents including ARBs (irbesartan, losartan), diuretics (hydrochlorothiazide), calcium channel blockers (amlodipine), and ACE inhibitors (ramipril, lisinopril).5,9,17,19–22 Only 1 of the comparative trials evaluated aliskiren at a dose of 37.5 mg daily.5 All other comparative studies evaluated aliskiren at doses of 75 to 600 mg daily (Table 2).5,9,17,19,20
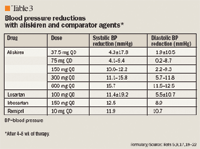
One large study comparing aliskiren with hydrochlorothiazide has been completed; however, this study is available only in abstract form, and data regarding the comparative efficacy of aliskiren and hydrochlorothiazide are not presented.19 The utility of adding hydrochlorothiazide to aliskiren 150 or 300 mg daily when patients do not respond to aliskiren alone was assessed. After 8 weeks of alis-kiren monotherapy, 45% of patients required the addition of hydrochlorothiazide for improved control. Blood pressure reduction with aliskiren plus hydrochlorothiazide was comparable to the reduction observed in those who responded to aliskiren alone.23
A study comparing the combination of amlodipine and aliskiren with each drug as monotherapy demonstrated that the addition of aliskiren to amlodipine 5 mg resulted in greater blood pressure reduction than that observed with amlodipine 5 mg alone and in a similar reduction to that observed with amlodipine 10 mg alone. However, low-dose amlodipine plus aliskiren was better tolerated than amlodipine 10 mg daily.21
Only 1 small study (N=27) has been reported in patients with heart failure.24 Patients included in this study were New York Heart Association class II and III, with an ejection fraction <35%. Patients were randomized to 6 weeks of treatment with ramipril (10 mg daily) or aliskiren (300 mg daily). Blood pressure reduction was similar between groups. No other clinical end points have been evaluated in patients with heart failure.
ADVERSE EVENTS
Aliskiren was generally well tolerated, requiring discontinuation in only 3.9% to 5% of patients.5,20 The most common adverse events occurring in studies of aliskiren included headache (2.4%–6.2%) and diarrhea (1.2%–11.4%).17,18 Diarrhea occurred in a dose-related fashion, with the highest incidence at the 600-mg dose.18 Less common adverse events included orthostasis, dizziness, fatigue, and weakness.5,17 With the exception of diarrhea at the highest dose of aliskiren, adverse events occurred at similar rates among patients treated with aliskiren, placebo, or an active comparator.
Aliskiren alone had effects on potassium concentrations similar to those of an ACE inhibitor and additive effects when used in combination with an ACE inhibitor. When aliskiren was combined with amlodipine 5 mg daily, patients experienced blood pressure control similar to that observed with amlodipine 10 mg daily but with less peripheral edema.21 Additionally, the incidence of cough occurring with an ACE inhibitor was reduced when the ACE inhibitor was combined with aliskiren.20 Patients in whom aliskiren was abruptly discontinued did not experience a rebound increase in blood pressure.7,8,10,17
DRUG INTERACTIONS

As with any antihypertensive agent, there is the potential for additive antihypertensive effect when aliskiren is used concomitantly with another agent that lowers blood pressure. However, hypotension was not a major concern when aliskiren was combined with ramipril, hydrochlorothiazide, or amlodipine in the clinical trials discussed previously.9,19–22
DOSING AND ADMINISTRATION
Dosing information for aliskiren is not yet available since the agent is currently under review by FDA. Given that the effects of aliskiren on angiotensin II, PRA, and ARC persist throughout a 24-hour period with doses >160 mg, it is likely that once-daily dosing will be used for hypertension. The high trough-to-peak ratio of the drug (63%–78%) also supports the use of once-daily dosing.17
Doses used in hypertension studies ranged from 37.5 to 600 mg daily.5,9,17,19,20,22 The lowest dose, 37.5 mg daily, did not produce a significant blood pressure reduction from baseline and therefore is not likely to be used clinically.5 When doses of 75 to 300 mg were used, the higher dose led to greater reductions in blood pressure and an increasing response rate, although in studies evaluating the 75-mg dose, blood pressure reductions were small and, in 1 study, were not substantially different from the reductions seen with the 37.5-mg dose.5,17–19 However, increasing the aliskiren dose to 600 mg daily has not produced increases in blood pressure reduction or response rate substantially higher than those observed with the 300-mg dose. In addition, gastrointestinal adverse events were more common with the 600-mg dose. Therefore, the doses to be used in patients with hypertension are likely to range from 150 to 300 mg daily.
The only study in patients with heart failure used a dose of 300 mg daily.24 Although this was a very small study, aliskiren was well tolerated. Therefore, future studies in patients with heart failure will likely employ doses from 150 to 300 mg as well.
In each issue, the "Focus on" feature reviews a newly approved or investigational drug of interest to pharmacy and therapeutics committee members. The column is coordinated by Robert A. Quercia, MS, RPh, clinical manager and director of Drug Information, Department of Pharmacy Services, Hartford Hospital, Hartford, Conn, and adjunct associate professor, University of Connecticut School of Pharmacy, Storrs, Conn; and by Craig I. Coleman, PharmD, assistant professor of pharmacy practice, University of Connecticut School of Pharmacy, and director, Pharmacoeconomics and Outcomes Studies Group, Hartford Hospital.
EDITORS' NOTE: The clinical information provided in "Focus on" articles is as current as possible. Due to regularly emerging data on developmental or newly approved drug therapies, articles include information published or presented and available to the author up until the time of the manuscript submission.
Dr Kalus is assistant professor of pharmacy practice, Eugene Applebaum College of Pharmacy and Health Sciences, Wayne State University, Detroit, Mich, and pharmacy clinical specialist in cardiology, Henry Ford Hospital, Detroit, Mich. He can be reached at jkalus@wayne.edu
Disclosure Information: The author reports no financial disclosures as related to products discussed in this article.
REFERENCES
1. Weber MA, Giles TD. Inhibiting the renin-angiotensin system to prevent cardiovascular diseases: Do we need a more comprehensive strategy? Rev Cardiovasc Med. 2006;7:45–54.
2. Stanton A. Therapeutic potential of renin inhibitors in the management of cardiovascular disorders. Am J Cardiovasc Drugs. 2003;3:389–394.
3. Lévy BI. Can angiotensin II type 2 receptors have deleterious effects in cardiovascular disease? Implications for therapeutic blockade of the renin-angiotensin system. Circulation. 2004;109:8–13.
4. Wood JM, Maibaum J, Rahuel J, et al. Structure-based design of aliskiren, a novel orally effective renin inhibitor. Biochem Biophys Research Comm. 2003;308:698–705.
5. Stanton A, Jensen C, Nussberger J, O'Brien E. Blood pressure lowering in essential hypertension with an oral renin inhibitor, aliskiren. Hypertension. 2003;42:1137–1143.
6. Azizi M, Ménard J, Bissery A, et al. Pharmacologic demonstration of the synergistic effects of a combination of the renin inhibitor aliskiren and the AT1 receptor antagonist valsartan on the angiotensin II-renin feedback interruption. J Am Soc Nephrol. 2004;15:3126–3133.
7. Nussberger J, Wuerzner G, Jensen C, Brunner HR. Angiotensin II suppression in humans by the orally active renin inhibitor aliskiren (SPP100): Comparison with enalapril. Hypertension. 2002;39:e1–e8.
8. Herron J, Mitchell J, Oh B, et al. The novel renin inhibitor aliskiren is not associated with rebound effects on blood pressure or plasma renin activity following treatment withdrawal. J Clin Hypertens. 2006;8(suppl A):A86. Abstract P-193.
9. Tschoepe D, Taylor A, Kilo C, et al. Aliskiren, alone and in combination with ramipril, significantly lowers blood pressure and plasma renin activity in patients with diabetes and hypertension, regardless of the degree of glycaemic control. Presented at: 42nd Annual Meeting of the European Association for the Study of Diabetes (EASD); September 14–17, 2006; Copenhagen–Malmoe, Denmark–Sweden. Abstract 0217.
10. Kilo C, Taylor A, Tschoepe D, Ibram G, Fang H, Prescott MF. Aliskiren, a novel renin inhibitor for treatment of hypertension, enhances renin system suppression by reducing plasma renin activity alone or in combination with ramipril in patients with diabetes. Eur Heart J. 2006;27(suppl):118–119. Abstract P789.
11. Pilz B, Shagdarsuren E, Wellner M, et al. Aliskiren, a human renin inhibitor, ameliorates cardiac and renal damage in double-transgenic rats. Hypertension. 2005;46:569–576.
12. Azizi M, Webb R, Nussberger J, Hollenberg NK. Renin inhibition with aliskiren: Where are we now, and where are we going? J Hypertens. 2006;24:243–256.
13. Feldman DL, Persohn E, Schutz H, et al. Renal localization of the renin inhibitor aliskiren. J Clin Hypertens. 2006;8(suppl A):A80. Abstract P-178.
14. Limoges D, Vaidyanathan S, Yeh C-M, Dieterich HA. Aliskiren, an orally effective renin inhibitor, shows dose linear pharmacokinetics in healthy volunteers. Clin Pharmacol Ther. 2006;79:P64. Abstract PIII-23.
15. Vaidyanathan S, Jermany J, Yeh CM, Bizot MN, Camisasca RP. Aliskiren, a novel orally effective renin inhibitor, exhibits similar pharmacokinetics and pharmacodynamics in Japanese and Caucasian subjects. Am J Hypertens. 2005;18 (suppl):A75–A76.
16. Zhao C, Vaidyanathan S, Yeh C-M, Dieterich HA. Pharmacokinetics and safety of the novel oral renin inhibitor aliskiren in patients with type 2 diabetes. Clin Pharmacol Ther. 2006;79:P12. Abstract PI-21.
17. Gradman AH, Schmieder RE, Lins RL, Nussberger J, Chiang Y, Bedigian MP. Aliskiren, a novel orally effective renin inhibitor, provides dose-dependent antihypertensive efficacy and placebo-like tolerability in hypertensive patients. Circulation. 2005;111:1012–1018.
18. Oh B-H, Chung J, Khan M, Keefe D, Satlin A. Aliskiren, an oral renin inhibitor, provides dose-dependent efficacy, and placebo-like tolerability in patients with hypertension. J Am Coll Cardiol. 2006;47(suppl A):370A–371A. Abstract 1027-191.
19. Villamil A, Chrysant S, Calhoun D, Schober B, Hsu H, Zhang J. The novel oral renin inhibitor aliskiren provides effective blood pressure control in patients with hypertension when used alone or in combination with hydrochlorothiazide. J Clin Hypertens. 2006;8(suppl A):A100. Abstract P-228.
20. Uresin Y, Taylor A, Kilo C, et al. Aliskiren, a novel renin inhibitor, has greater BP lowering than ramipril and additional BP lowering when combined with ramipril in patients with diabetes and hypertension. J Hypertens. 2006;24(suppl 4):S82. Abstract P4.269.
21. Munger MA, Drummond W, Essop MR, Maboudian M, Khan M, Keefe DL. Aliskiren as add-on to amlodipine provides significant additional blood pressure lowering without increased oedema associated with doubling the amlodipine dose. Eur Heart J. 2006;27(suppl):117. Abstract P784.
22. Strasser RH, Puig JG, Farsang C, Kroket M, Li J, van Ingen H. The oral direct renin inhibitor aliskiren has comparable safety and efficacy to lisinopril in patients with severe hypertension. Presented at: 21st Scientific Meeting of the International Society of Hypertension; October 15–19, 2006; Fukuoka, Japan. Poster PM1-01-01.
23. Sica D, Gradman A, Lederballe O, Meyers M, Cai J, Keefe DL. Aliskiren, a novel renin inhibitor, is well tolerated and has sustained BP-lowering effects alone or in combination with HCTZ during long-term (52 weeks) treatment of hypertension. Eur Heart J. 2006;27(suppl):121. Abstract P797.
24. Seed A, Gardner R, McMurray J, et al. First experience with an orally active renin inhibitor (aliskiren) in patients with chronic heart failure. Heart. 2003;89(suppl 1):A57. Abstract 192.
25. Dieterle W, Corynen S, Mann J. Effects of the oral renin inhibitor aliskiren on the pharmacokinetics and pharmacodynamics of a single dose of warfarin in healthy subjects. Br J Clin Pharmacol. 2004;58:433–436.
26. Dieterle W, Corynen S, Mann J. Pharmacokinetic interactions of the oral renin inhibitor aliskiren with lovastatin, atenolol, celecoxib and cimetidine. Int J Clin Pharmacol Ther. 2005;43:527–535.
27. Kemp C, Vaidyanathan S, Yeh C-M, Dieterich HA. Aliskiren, the first in a new class of orally effective renin inhibitors, has no clinically significant drug interactions with digoxin in healthy volunteers. Clin Pharmacol Ther. 2006;79:P64.
28. Kemp C, Vaidyanathan S, Yeh C-M, Dieterich HA. Pharmacokinetic interaction of the oral renin inhibitor aliskiren with hydrochlorothiazide in healthy volunteers. Clin Pharmacol Ther. 2006;79:P12.
FDA Approves Combination Therapy for Pulmonary Arterial Hypertension
March 25th 2024J&J’s Opsynvi is single-tablet combination of macitentan, an endothelin receptor antagonist, and tadalafil, a PDE5 inhibitor. It will be priced on parity with Opsumit, which is also a J&J product to treat patients with PAH.
FDA Issues Complete Response Letter for Onpattro in Heart Failure Indication
October 9th 2023Alnylam Pharmaceuticals will no longer pursue this indication of Onpattro and will instead on focus on a label expansion for Amvuttra, which is in phase 3 development to treat patients with cardiomyopathy of ATTR amyloidosis.
