- Safety & Recalls
- Regulatory Updates
- Drug Coverage
- COPD
- Cardiovascular
- Obstetrics-Gynecology & Women's Health
- Ophthalmology
- Clinical Pharmacology
- Pediatrics
- Urology
- Pharmacy
- Idiopathic Pulmonary Fibrosis
- Diabetes and Endocrinology
- Allergy, Immunology, and ENT
- Musculoskeletal/Rheumatology
- Respiratory
- Psychiatry and Behavioral Health
- Dermatology
- Oncology
Aspirin plus esomeprazole superior to clopidogrel for prevention of recurrent ulcer bleeding
Among patients with a history of aspirin-induced ulcer bleeding, aspirin plus esomeprazole was shown to be superior to clopidogrel for the prevention of recurrent bleeding. The results of a 12-month, prospective, randomized, double-blind trial do not support current American College of Cardiology/American Heart Association guidelines recommending that clopidogrel be used as an alternative antiplatelet agent in patients who have a major gastrointestinal intolerance to aspirin, according to the authors of the study.
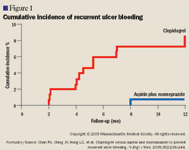
"Our results raise doubts about the gastrointestinal safety of clopidogrel even in the absence of active ulcers," the authors stated.
The study, conducted in Hong Kong, enrolled 320 patients who had been taking low-dose aspirin (≤325 mg/d) to prevent vascular diseases and who presented with upper gastrointestinal (GI) bleeding. Patients with Helicobacter pylori infection were treated for 1 week with a 3-drug regimen that included a proton pump inhibitor (PPI). During this period, aspirin was withheld. All patients received PPIs to promote the healing of ulcers. Patients were considered eligible for study inclusion if, after 8 weeks, an endoscopy confirmed that their ulcers had healed and they tested negative for H pylori.
The end point of recurrent ulcer bleeding occurred in 13 patients (8.6%; 6 gastric ulcers, 5 duodenal ulcers, 2 both) (95% CI, 4.1%–13.1%) who received clopidogrel, compared with 1 patient (0.7%; 1 duodenal ulcer) (95% CI, 0%–2.0%) who received aspirin plus esomeprazole (95% CI for the difference, 3.4–12.4; P=.001). Researchers regarded the recurrent ulcer bleeding in the clopidogrel recipients as "unacceptably high." In 10 of the 14 patients with recurrent bleeding (71.4%), the ulcers appeared at their previous locations.
Adverse events occurred in 9.4% of those who received clopidogrel (7.5% had dyspepsia and 1.9% had allergy) and in 4.4% of those who received aspirin plus esomeprazole (2.5% had dyspepsia and 1.9% had allergy). Recurrent ischemic events occurred in 9 patients who received clopidogrel (6 had unstable angina, 1 had a myocardial infarction [MI], and 2 had cerebrovascular insufficiency) and in 11 patients who received aspirin plus esomeprazole (7 had unstable angina, 1 had an MI, and 3 had cerebrovascular insufficiency).
In an accompanying editorial, Byron Cryer, MD, noted study limitations, including the fact that all of the patients were negative for or had been cured of H pylori infection, and none were taking anticoagulants or corticosteroids during the study, suggesting that the results cannot be applied with certainty to patients at risk for GI complications of aspirin therapy.
Dr Cryer, associate professor of Medicine at the University of Texas Southwestern Medical School, also commented: "Although clopidogrel and other agents that impair angiogenesis might not be the primary cause of gastrointestinal ulcers, their antiangiogenic effects may impair the healing of background ulcers; when combined with the propensity to increase bleeding, these agents may convert small, silent ulcers into large ulcers that bleed profoundly."
SOURCES Chan FK, Ching JY, Hung LC, et al. Clopidogrel versus aspirin and esomeprazole to prevent recurrent ulcer bleeding. N Engl J Med. 2005;352:238–244.
Cryer B. Reducing the risks of gastrointestinal bleeding with antiplatelet therapies. N Engl J Med. 2005;352:287–289.
Coalition promotes important acetaminophen dosing reminders
November 18th 2014It may come as a surprise that each year Americans catch approximately 1 billion colds, and the Centers for Disease Control and Prevention estimates that as many as 20% get the flu. This cold and flu season, 7 in 10 patients will reach for an over-the-counter (OTC) medicine to treat their coughs, stuffy noses, and sniffles. It’s an important time of the year to remind patients to double check their medicine labels so they don’t double up on medicines containing acetaminophen.
Support consumer access to specialty medications through value-based insurance design
June 30th 2014The driving force behind consumer cost-sharing provisions for specialty medications is the acquisition cost and not clinical value. This appears to be true for almost all public and private health plans, says a new report from researchers at the University of Michigan Center for Value-Based Insurance Design (V-BID Center) and the National Pharmaceutical Council (NPC).
Management of antipsychotic medication polypharmacy
June 13th 2013Within our healthcare-driven society, the increase in the identification and diagnosis of mental illnesses has led to a proportional increase in the prescribing of psychotropic medications. The prevalence of mental illnesses and subsequent treatment approaches may employ monotherapy as first-line treatment, but in many cases the use of combination of therapy can occur, leading to polypharmacy.1 Polypharmacy can be defined in several ways but it generally recognized as the use of multiple medications by one patient and the most common definition is the concurrent use of five more medications. The presence of polyharmacy has the potential to contribute to non-compliance, drug-drug interactions, medication errors, adverse events, or poor quality of life.
Medical innovation improves outcomes
June 12th 2013I have been diagnosed with stage 4 cancer of the pancreas, a disease that’s long been considered not just incurable, but almost impossible to treat-a recalcitrant disease that some practitioners feel has given oncology a bad name. I was told my life would be measured in weeks.
