- Safety & Recalls
- Regulatory Updates
- Drug Coverage
- COPD
- Cardiovascular
- Obstetrics-Gynecology & Women's Health
- Ophthalmology
- Clinical Pharmacology
- Pediatrics
- Urology
- Pharmacy
- Idiopathic Pulmonary Fibrosis
- Diabetes and Endocrinology
- Allergy, Immunology, and ENT
- Musculoskeletal/Rheumatology
- Respiratory
- Psychiatry and Behavioral Health
- Dermatology
- Oncology
Biologic therapies for the treatment of chronic plaque psoriasis
Psoriasis is a chronic, inflammatory dermatologic disease that can have a significant physical and psychological impact on affected patients.
Abstract Psoriasis is a chronic, inflammatory dermatologic disease that can have a significant physical and psychological impact on affected patients. Traditional therapies have provided varying degrees of efficacy in psoriasis management. The most effective treatments have been characterized by underutilization, inconvenience, and adverse events, making long-term management challenging. Ideally, psoriasis therapy should be easily administered and should result in the tolerable and efficacious management of symptoms, while reducing the time and costs associated with visits to health-care providers. Several new classes of biologic therapies designed to block the function of specific molecules involved in the psoriatic inflammatory process have come closer to achieving these goals. (Formulary. 2005;40:184-199.)
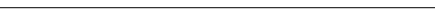
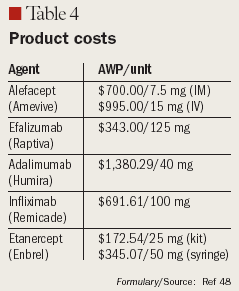
Psoriasis is a chronic skin disorder of variable severity that affects 1% to 3% of the worldwide population and more than 6 million people in the United States.1-3 It affects men and women equally and typically manifests during the third decade of life, though it can occur at any age. It is well-established that the disease negatively impacts mental, physical, and social well-being, with a reduction in quality of life that is comparable to that seen with major chronic conditions such as diabetes, heart disease, and cancer.4
There are 5 types of psoriasis: plaque type or psoriasis vulgaris, guttate, pustular, inverse, and erythrodermic.6 Eighty-five percent to 90% of psoriasis cases are chronic plaque psoriasis, which is characterized by chronic localized scaly erythematous plaques that may affect any area of the body but are predisposed to the scalp, knees, elbows, and lumbosacral area. The scales are silvery-white in appearance, can vary in density and size, and reveal bleeding points when removed. Pruritis is reported in 20% of cases, but generally the scales are otherwise asymptomatic. The plaques are more emotionally than physically disabling.
Psoriatic exacerbations may be triggered by factors such as emotional stress, skin injury, and certain medications such as lithium, beta-blockers, and antimalarials. Severity is measured both by the extent of the disease and the impact on quality of life. Mild-to-moderate disease affects less than 20% of the body surface area, while more than 20% involvement is considered severe.7 However, smaller areas of disease (eg, palms, soles, head, genitalia) that significantly interfere with quality of life may also be considered severe.6 Approximately one-third of patients with chronic plaque psoriasis have moderate-to-severe disease.8 Treatment is long-term and individualized, with the ultimate goal of achieving and maintaining complete remission.6,7
PATHOGENESIS Psoriasis appears to be triggered by the recognition of unidentified antigens in the dermis by antigen-presenting cells (APCs). APCs migrate to the lymph nodes, where they interact with naïve T-cells through a variety of cell surface proteins, thereby activating the T-cells to specifically recognize the initiating antigen.
These activated T-cells proliferate, enter the circulation, and migrate through the endothelium into the dermis in response to inflammatory cytokines. In the dermis, activated T-cells play an integral role in the local inflammatory response by secreting several cytokines, including TNF, interferon-γ, and interleukin-2.9 Inflammatory cytokines propagate the inflammatory response by promoting synthesis of other cytokines and inflammatory mediators. These include adhesion molecules (eg, intracellular cell adhesion molecule [ICAM]), vascular endothelial growth factors, matrix metalloproteases, and prostaglandins.10 This cascade of inflammatory events contributes to the local hyperproliferation of keratinocytes, which is a key step in the development of psoriatic lesions.9

HISTORICAL THERAPIES The treatment of psoriasis focuses on decreasing the severity and extent of the disease to a level that no longer interferes with daily living and quality of life. Traditional treatments have included topical therapy (eg, coal tar-based products, moisturizing lotions, topical steroids) for mild disease, and systemic therapy (eg, oral retinoids, cyclosporine, and methotrexate) and phototherapy for more widespread or moderate-to-severe disease.
Both phototherapy and systemic therapy are highly effective; however, they are also associated with side effects. Phototherapy, which involves the exposure of lesions to ultraviolet light, may cause premature aging of skin and may increase the risk of squamous cell carcinoma and other skin cancers when used at very high doses.8 Combining phototherapy with other systemic therapies, such as retinoids or methotrexate, may reduce the risk for malignancy. Phototherapy must be administered at a licensed facility, requires multiple visits, and must be administered under the supervision of a dermatologist.
As described below, systemic therapies may be toxic with both short- and long-term use. An estimated two-thirds of American dermatologists rarely prescribe these agents due to the potential for serious toxicities.11
TYPES Oral retinoids are vitamin A derivatives that have anti-inflammatory, antikeratinizing, and antiproliferative effects on the skin. Acitretin, a second-generation retinoid, is the only oral retinoid currently available in the United States. The clinical studies involving oral retinoids are markedly heterogeneous in size, baseline disease type and severity, concomitant medications used, and duration of treatment. It appears, however, that retinoid monotherapy at doses of 10 to 50 mg/d is moderately effective in treating the symptoms of psoriasis, clearing more than 75% of plaques in up to 60% of treated patients. When used in conjunction with phototherapy, lower doses (10–25 mg/d) may be used.12 Combination therapy is more effective than either treatment alone, with clearance rates of 96% for combination therapy compared with 80% for phototherapy alone, and is associated with reduced risk of toxicity from either treatment.12,13
Retinoids are associated with dose-related mucocutaneous side effects (eg, cheilitis, hair loss), hyperlipidemia, hepatoxicity, and inherent teratogenicity, which limit their use in women of child-bearing potential.14 Due to the long half-life of one of its active metabolites (etretinate), women taking acitretin must use 2 forms of contraception during therapy and for 3 years after cessation of therapy.15
Cyclosporine and methotrexate are both highly effective immunosuppressant therapies for chronic plaque psoriasis, although their use is often limited by nephrotoxicity and hepatotoxicity, respectively. Cyclosporine and methotrexate have comparable efficacy, producing at least 75% improvement from baseline in 60% to 70% of patients with moderate-to-severe psoriasis within 16 weeks.16 Symptoms will relapse within weeks of discontinuation, so chronic therapy is often necessary. To minimize the risk for cumulative toxicities, cyclosporine and methotrexate are often rotated at regular intervals with other psoriasis treatments.
Up to 20% of patients receiving cyclosporine for psoriasis will exhibit signs of renal impairment (eg, elevated creatinine and BUN concentrations). Renal tubular atrophy and interstitial fibrosis have also been reported in patients who received cyclosporine at a mean dosage of 3 mg/kg daily for an average of 5 years.17 In addition to dose-related renal toxicity, nearly one-third of patients receiving cyclosporine for the treatment of psoriasis will develop hypertension (SBP>160 or DBP>90) and nervous system effects (eg, headache, paresthesias). Dermatologic reactions (eg, hypertrichosis, gingival hyperplasia) have also occurred in about 18% of patients being treated for psoriasis.17
Chronic hepatotoxicity associated with methotrexate typically occurs after prolonged therapy (>2 years) and cumulative doses of 1.5 grams or more. Additional adverse effects of methotrexate therapy for psoriasis include erythematous rashes, dermatitis, and alopecia. Burning and erythema in psoriatic areas may occur for 1 to 2 days following each dose. Up to 5% of patients will experience photosensitivity. Cases of severe cutaneous reactions, such as Stevens-Johnsons syndrome and toxic epidermic necrolysis, have been reported. Patients should be monitored for pulmonary fibrosis and interstitial pneumonitis, as well as hematologic abnormalities such as leukopenia, thrombocytopenia, anemia, and hemorrhage.17,18 In addition, monitoring of renal function is required, as renal impairment may lead to accumulation of the drug. For the treatment of psoriasis, the total weekly dose of methotrexate should not exceed 30 mg. Methotrexate is both an abortifacient and teratogenic; therefore, it is contraindicated in pregnancy.
Combining phototherapy with either cyclosporine or methotrexate maintains efficacy and allows for lower total cumulative doses, thereby reducing the individual toxicities associated with each agent.14
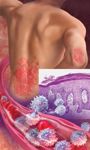
T-CELL AGENTS T-cell agents were the first biologics to receive FDA approval for the treatment of chronic plaque psoriasis.
Alefacept. Alefacept (Amevive, Biogen) was approved by FDA in January 2003 for the treatment of moderate-to-severe chronic plaque psoriasis in adult patients who are candidates for systemic therapy or phototherapy.20
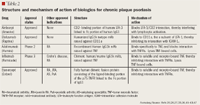
The second pathway involves reducing the total number of T-cells. Alefacept reduces the total subset of CD2+ T-cells, presumably by providing a bridging mechanism that links T-cells (via the CD2 moiety) to Fc receptors, which are present on the surface of cytotoxic leukocytes (Table 2).
Overall improvements in psoriasis symptoms were observed as measured by the PASI 75, PASI 50, and Physician's Global Assessment (PGA). Throughout the treatment period, 33% of patients receiving alefacept 15 mg IM achieved a PASI 75 response, compared to 13% of those receiving placebo (P<.001). Approximately 57% of patients receiving alefacept 15 mg IM achieved a PASI 50 response, compared to 35% receiving placebo (P<.001).21 The overall response rates as measured by PGA scores were considered "clear" or "almost clear" for 24% of patients receiving alefacept 15 mg and 8% of those receiving placebo (P<.001).
The effectiveness and safety of repeat IV alefacept courses have also been studied in two phase 3 extension trials and one phase 2 open-label extension trial.22-24 Patients who were enrolled in the initial phase 2 and 3 clinical trials were eligible to receive retreatment upon meeting study inclusion criteria. Each study evaluated the effects of alefacept for 12 weeks, followed by a 12-week observation period, and then retreatment with another course of alefacept for another 12 weeks. Although each study used varying repeat doses (7.5 mg/7.5 mg IV, 15 mg/15 mg IM, and 0.150 mg/kg/7.5 mg IV), all of the data suggested additional reductions in PASI 50, PASI 75, and PGA scores beyond those observed following a single alefacept course.
Two repeated treatment courses of alefacept 15 mg IM once weekly for 12 weeks improved the PASI 50 score from a 57% reduction to a 69% reduction at the conclusion of therapy.24 Similar improvements were observed in PGA scores with 24% vs 31% of those achieving a "clear" to "almost clear" score following one and two alefacept 15 mg IM once weekly courses, respectively.
Dose-dependent reductions in circulating CD4+ and CD8+ T-lymphocytes were the most common reason for therapy discontinuation.20 This dose-dependent lymphopenia has been attributed to the clinical activity of alefacept, whereby alefacept reduces CD4+ and CD8+ memory T-cells and does not affect naïve T-cells.25 As a result of this dose-dependent reduction in CD4+ and CD8+ memory T-cells, baseline and weekly monitoring of lymphocyte counts is recommended. Alefacept must be withheld when T-lymphocytes decrease beyond 250 cells/L. Treatment should be discontinued if the counts remain below 250 cells/L for 1 month.
A second treatment cycle may be given if the CD4+ T-lymphocyte count is greater than 250 cells/L and 12 weeks have elapsed since the previous cycle. There are limited data on the effect of retreatment beyond 2 cycles.20
To avoid the risk of excessive immunosuppression, alefacept should not be combined with phototherapy or other immunosuppressants. Approximately 1.8% of patients in clinical trials developed malignancies (basal or squamous cell cancers and lymphoma).14 Three percent of patients receiving alefacept developed low-titer antibodies to alefacept; however, no correlation between antibody development and clinical response or adverse effects has been determined.14 No formal drug interaction studies with alefacept have been performed.20
Efalizumab. Efalizumab (Raptiva, Genentech) was approved by FDA in October 2003 for the treatment of moderate-to-severe chronic plaque psoriasis in adults who are candidates for systemic therapy or phototherapy.26
In all 4 studies, patients were randomized to receive weekly SC doses of either efalizumab (1 mg/kg or 2 mg/kg) or placebo for 12 weeks. An initial conditioning efalizumab dose of 0.7 mg/kg was administered to patients receiving efalizumab (to prevent first-dose-related reactions) before the delivery of subsequent doses. Between 22% and 39% of patients receiving 1 mg/kg efalizumab, compared with 2% to 5% of those receiving placebo, achieved a PASI 75 response after 12 weeks of treatment (P<.001).26
In addition, 52% to 59% of treated patients achieved PASI 50 compared with 14% to 16% of those receiving placebo (P<.001).29 A significantly higher percentage of patients treated with efalizumab also obtained "minimal" to "clear" Overall Lesion Severity (OLS), "clear" or "almost clear" PGA, and had higher mean percentage improvements from baseline in Dermatology Life Quality Index (DLQI), itching Visual Analog Scale (VAS) and Psoriasis Symptom Assessment (PSA) scores relative to placebo (P<.001 for all measures).29 The time to symptom relapse (defined as a loss of 50% improvement in PASI) ranged from a median of 67 to 84 days after discontinuing treatment and occurred in 67% to 83% of patients studied.28,29
Continuous efalizumab treatment for 24 weeks appears to be effective for achieving PASI 75 response in patients who were initial nonresponders after 12 weeks of therapy. In a randomized, double-blind, placebo-controlled study involving 556 patients, 26.6% of efalizumab (1 mg/kg/wk) recipients achieved PASI 75 response after 12 weeks of treatment. After 24 weeks of treatment, the response rate increased to 43.8%.30 In 2 open-label extension studies, patients who responded to treatment after 12 weeks were re-randomized to receive either efalizumab or placebo for an additional 12 weeks. A higher proportion of patients in the efalizumab group maintained PASI 75 during the extended treatment course relative to patients receiving placebo, though the response rates varied widely between the studies: 77% versus 20% (P<.001) in one study, and 20% versus 7% (P=.018) in the other study.29,31
An open-label, late phase 3 study has evaluated up to 3 years of efalizuamb therapy (1 mg/kg/wk) for patients with moderate-to-severe chronic plaque psoriasis.32 Among 290 patients who entered the maintenance phase, 51% to 56% of patients were PASI-75 responders throughout the follow-up. A total of 146 patients completed 33 months of maintenance therapy, and up to 75% of these patients maintained PASI 75 response toward the end of the study. There was no evidence of cumulative toxic effects with long-term efalizumab treatment.29,31,32
Intermittent efalizumab therapy does not appear to be as effective as continuous therapy. In a 12-week open-label extension study of efalizumab, patients who had previously responded to a 12-week course of efalizumab were observed off-treatment until relapse, after which time they were retreated with efalizumab. Only 31% of these initial responders re-established PASI 75 with retreatment.28
Efalizumab suppresses the immune system and may consequently increase the risk of infection and malignancy. Efalizumab should be used with caution in patients with a chronic infection or history of recurrent infections and in those who are at high risk for or have a history of malignancy. Patients should not receive vaccines while taking efalizumab.26,28
Worsening psoriasis, as well as conversion to psoriatic erythroderma and pustular psoriasis, have been observed in patients following discontinuation of efalizumab therapy. Some of these patients required hospitalization and alternative antipsoriatic therapy to manage worsening disease. Alternate therapy should be administered following the conclusion or temporary discontinuation of efalizumab.
Elevated transaminases, reversible transient elevated eosinophils, lymphocytes, and white blood cell count, as well as development of neutralizing antibodies (6.3% incidence), have been observed in clinical trials of patients taking efalizumab. The long-term effects of efalizumab immunogenicity are not known.26
To avoid the risk of excessive immunosuppression, efalizumab should not be combined with phototherapy or other immunosuppressants.26
MONOCLONAL TNF ANTIBODIES Several TNF inhibitors are under investigation for the treatment of psoriasis.
Adalimumab. Adalimumab (Humira, Abbott Laboratories) is currently undergoing phase 2 studies for the treatment of chronic plaque psoriasis. Adalimumab is FDA-approved for the treatment of symptoms and progression of rheumatoid arthritis (RA) in adult patients aged more than 18 years.
The primary efficacy end point was the percentage of patients achieving a PASI 75 response at Week 12. At Week 12, significantly more patients receiving adalimumab every other week (53%) or once weekly (80%) achieved a PASI 75 response, compared with those receiving placebo (4%).34 The preliminary findings of a 48-week extension phase of this study have also been presented. After 24 weeks of continuous adalimumab treatment, 67% of patients receiving adalimumab every other week and 77% of patients receiving weekly treatment had a PASI 75 response. Furthermore, 44% and 66% of the every other week and weekly treatment arms, respectively, achieved a PASI 90 response or better.35
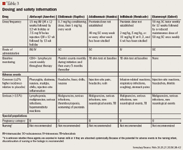
Experience in patients with rheumatoid arthritis (RA) has indicated the necessity to observe several precautions during adalimumab therapy. The possibility of an increased risk of tuberculosis (TB) has been observed in clinical trials (0.6% incidence) and through post-marketing surveillance.33 These observations led to a black box warning that requires a tuberculin skin test before initiation of adalimumab therapy (Table 3).

The development of neutralizing antibodies has been observed following adalimumab treatment. Concomitant methotrexate therapy reduced the incidence of these antibodies in patients receiving adalimumab for RA. Although more studies in patients with psoriasis are needed, the existing evidence suggests that concomitant methotrexate therapy may be used and may be useful to preserve adalimumab efficacy over time.33
Infliximab. Infliximab (Remicade, Centocor) is currently in phase 3 trials for the treatment of chronic plaque psoriasis. Infliximab is currently FDA-approved as monotherapy for the treatment of Crohn's disease (CD), ankylosing spondylitis and psoriatic arthritis, and in combination with methotrexate for the treatment of RA.
For FDA-approved indications, infliximab carries a black box warning that severe, rarely fatal, TB-invasive fungal infections and other opportunistic infections have been observed in patients receiving infliximab.36 In 2002, the estimated rate of TB reported to FDA for the first year of therapy with infliximab in the United States was approximately 0.4% of patients treated for RA and 0.09% of patients treated for CD.37
All patients being considered for infliximab therapy should be evaluated for active or latent TB infection.36 Likewise, patients should be advised to seek medical attention if they experience symptoms suggestive of tuberculosis while taking the drug. The drug should be avoided in patients with active infection and used with caution in patients with a history of recurrent infection. Infliximab is contraindicated in patients with moderate-to-severe (New York Heart Association [NYHA] class III/IV, left ventricular ejection fraction <35%) heart failure (HF), due to the significantly higher incidence of hospitalization and death due to worsening HF symptoms in patients treated with infliximab during clinical trials. Infliximab should be discontinued in patients who develop or experience worsening HF.36 Infliximab should be used with caution in patients with mild heart failure (NYHA class I/II).36

Infliximab may trigger complement-mediated lysis of TNF-alpha-expressing cells in vitro. The clinical implications of this activity in vivo are not known. Several cell types, such as monocytes and activated T-cells, express membrane-bound TNF; destruction of these cells may dampen the immune response to improve clinical symptoms but may also increase risk for infection.36
The primary end point was the proportion of patients achieving PASI 75 at Week 10. Compared to placebo, a higher percentage of infliximab recipients achieved PASI 75 at Week 10 (72% of the low-dose group, 86% of the high-dose group, and 6% of the placebo group; P<.001 for both treatment groups compared with placebo).38
Thirty-three patients with moderate-to-severe plaque psoriasis [baseline PASI 10–43] were enrolled in another randomized, double-blind, placebo-controlled trial of infliximab monotherapy for plaque psoriasis. Patients with at least 5% BSA involvement were randomized to receive either infliximab (5 mg/kg or 10 mg/kg) or placebo at Weeks 0, 2, and 6, followed by assessment at Week 10. The mean baseline PASI score ranged from 20.3 to 26.6 among the treatment groups. The primary efficacy end point was a PGA rating of "good," "almost clear," or "clear" at Week 10. This was achieved in 82% and 91% of the infliximab 5 mg/kg and 10 mg/kg groups, respectively. Only 18% of placebo recipients attained this end point (P=.0089 for 5 mg/kg vs placebo; P=.0019 for 10 mg/kg vs placebo). The secondary end point, PASI 75, was achieved in 82% and 73% of the infliximab 5 mg/kg and 10 mg/kg groups, respectively, compared with 18% of patients in the placebo group (P=.0089 for 5 mg/kg vs placebo; P=.03 for 10 mg/kg vs placebo). Significant mean percentage improvements in PASI score from baseline were evident by Week 2 of therapy for both treatment groups compared with placebo. The median time to response was 4 weeks.39
In an open-label extension of the same study (Weeks 10 through 26), 29 patients who had responded to infliximab induction therapy were evaluated for time to relapse and efficacy of retreatment. Thirty-one percent of patients experienced relapse between Weeks 22 and 34. Retreatment improved PASI scores, but not to the extent seen with the initial course of therapy. Loss of response began at Week 14 in the 5mg/kg group and Week 18 in the 10 mg/kg group. Forty percent of patients in the 5 mg/kg group and 73% of patients in the 10 mg/kg group maintained a PASI 50 response from the end of therapy through Week 26. Additionally, 33% and 67% of patients in the 5 and 10 mg/kg treatment groups, respectively, sustained a PASI 75 response through Week 26.40
Other adverse events that occurred in more than 5% of patients studied included headache, pruritus, fatigue, myalgia, pain, back pain, and infections (ie, upper respiratory tract infection, sinusitis, pharyngitis).38
Positive antinuclear antibody titers developed in 2 infliximab-treated (5 mg/kg) patients after 10 weeks of treatment. Neither patient had lupus or lupus-like symptoms and both responded well to treatment.39 The incidence of ANAs and anti-double stranded DNA antibodies has occurred in 52% and 17% of patients receiving therapeutic doses of infliximab for RA and CD, respectively, compared to 19% and 0% of those patients receiving placebo. The development of neutralizing antibodies may lead to a reduction in efficacy and increases the likelihood of infusion-related reactions.36 The development of lupus-like syndromes, however, appears to be rare.
To avoid the risk of excessive immunosuppression, infliximab should be used with caution when combined with other immunosuppressants.36
SOLUBLE TNF RECEPTOR INHIBITORS The recognition that t-cells and inflammatory cytokines are important in the pathogenesis of psoriasis created a new therapeutic option for biologic agents called soluble tnf receptor inhibitors. Soluble tnf receptor inhibitors prevent interactions with cell surface receptors and help reduce inflammation within plaques. Only one soluble tnf receptor inhibitor is currently approved for treatment of chronic plaque psoriasis, and it is the most widely used biologic agent in the United States.11
Etanercept. Etanercept (Enbrel, Amgen/Wyeth/Immunex) was approved by FDA in April 2004 for the treatment of adult patients with moderate-to-severe chronic plaque psoriasis who are candidates for systemic therapy or phototherapy.41
Etanercept is supplied as a lyophi-lized powder for parenteral administration following reconstitution with supplied water.

No dose-related increases in adverse events or infections were observed. The following adverse events were reported in greater than 10% of patients with chronic plaque psoriasis and occurred at a frequency greater than placebo: upper respiratory tract infections, headache, rhinitis, injection-site bruising, sinusitis, hypertension, and accidental injury.44 There were no opportunistic infections or TB cases reported.44,45 Non-neutralizing antibodies have been detected in patients receiving etanercept for RA.41,45 Depending on the method used to detect autoantibodies (Crithidia luciliae assay or radioimmunoassay), nearly 3% to 15% of patients using etanercept for RA developed positive antibodies.41 Eight out of 486 (1.6%) patients receiving etanercept for psoriasis developed antibodies.41,45 The effects of non-neutralizing antibody development on efficacy or adverse events has not been determined.41
Etanercept may be combined with phototherapy or other systemic immunosuppressants (eg, methotrexate) if clinically necessary. To avoid the risk of excessive immunosuppression, etanercept should be used with caution when combined with other immunosuppressants.41 In some patients, serious infections have occurred when etanercept was used alone or in combination with other immunosuppressants. For example, approximately 7% of RA patients receiving etanercept and anakinra (human interleukin-1 receptor antagonist) therapy developed serious infections as compared with patients receiving etanercept alone (0%).41 Etanercept should be avoided in patients with active infection and used with caution in patients with a history of recurrent infection. If a serious infection or sepsis develops during therapy, etanercept should be discontinued.41
FORMULARY CONSIDERATIONS FDA-approved agents for the treatment of chronic plaque psoriasis include alefacept, efalizumab, and etanercept. All 3 biologics are effective in reducing the severity and extent of disease. Efalizumab and etanercept were effective at maintaining improvements after 24 weeks of continuous therapy. Alefacept has also sustained therapeutic effects following two 12-week courses separated by a 12-week observation period. The optimal durations of therapy for all of the biologics have yet to be defined.
Among the various injectable methods of administration, the SC route appears to be the most convenient and does not involve the inconvenience and cost of extra medical office visits for IV drug administration. With proper training and education, patients may self-administer SC injections at home. Etanercept and efalizumab are available for SC injection, while alefacept may be administered as an IV bolus or as an IM injection.

To date, no clinical trials have directly compared biologic agents to traditional systemic therapies for the treatment of psoriasis. Additionally, there are no head-to-head trials comparing the various biologic agents for the treatment of chronic plaque psoriasis. Furthermore, despite the standardized psoriasis rating scales used in clinical trials, comparing biologics is difficult due to variations in baseline disease characteristics and disease severity. It appears, however, that these newer agents are less effective than cyclosporine, methotrexate, or PUVA administered at optimal doses but may offer a better long-term safety profile.
Until further studies are conducted comparing the various treatments for chronic plaque psoriasis, the role of biologic agents on the formulary remains unclear. Currently, both adalimumab and infliximab are in development for plaque psoriasis and have demonstrated some promising results. In particular, infliximab appears to demonstrate more significant reductions in disease severity compared with other biologics, though this needs to be confirmed in head-to-head studies.
More studies are ongoing in psoriasis patients. The results from these studies, as well as the results from studies of other biologics, must be taken into account before formulary decisions can be made. Relative to systemic therapies and phototherapy, however, biologics represent a significant advancement in psoriasis treatment because they are efficacious and do not appear to carry the risk of cumulative toxicities.
Dr Tsourounis is director, Drug Information Analysis Service, and associate professor of clinical pharmacy at the University of California San Francisco (UCSF) School of Pharmacy, San Francisco, Calif. She can be reached at tsourounisc@pharmacy.ucsf.edu
. Dr Cheng is clinical pharmacist, Drug Information Analysis Service, and assistant clinical professor at the UCSF School of Pharmacy. The preparation of this article was supported in part by an unrestricted educational grant from Amgen Inc.
REFERENCES 1. Lebwohl M. Psoriasis. Lancet. 2003;361:1197–1204.
2. Tutrone WD, Kagen MH, Barbagallo J, Weinberg JM. Biologic therapy for psoriasis: a brief history, II. Cutis. 2001;68:367–372.
3. Koo J, Lee E, Lee CS, Lebwohl M. Psoriasis.J Am Acad Dermatol. 2004;50:613–622.
4. Rapp SR, Feldman SR, Exum ML, et al.Psoriasis causes as much disability as other major medical diseases. J Am Acad Dermatol. 1999; 41:401–407.
5. Krueger G, Koo J, Lebwohl M, et al. The impact of psoriasis on quality of life: results of a 1998 National Psoriasis Foundation patient-membership survey. Arch Dermatol. 2001;137:280-284.
6. Frequently Asked Questions About Psoriasis. The National Psoriasis Foundation website. Available at: http:// http://www.psoriasis.org/. Accessed May 27, 2005.
7. Ellsworth A. Psoriasis. In: Koda-Kimble M, Young L, Kradjan W, Guglielmo BJ, eds. Applied Therapeutics: The Clinical Use of Drugs. 8th ed. Philadelphia: Lippincott Williams and Wilkins; 2005:40.1–40.15.
8. FDA Center for Drug Evaluation and Research. Food and Drug Administration website. Available at: http:// http://www.fda.gov/ohrms/dockets/ac/02/slides/3865S1_01_fda-bonvini/. Accessed May 27, 2005.
9. Mehlis SL, Gordon KB. The immunology of psoriasis and biologic immunotherapy. J Am Acad Dermatol. 2003;49:S44–S50.
10. Lebwohl M, Ali S. Treatment of psoriasis. Part 2. Systemic therapies. J Am Acad Dermatol. 2001;45:649–661.
11. Koo J, Khera P. Update on the mechanisms and efficacy of biological therapies for psoriasis.J Dermatol Sci. 2005;38:75–87.
12. Lebwohl M, Ali S. Treatment of psoriasis. Part 1. Topical therapy and phototherapy. J Am Acad Dermatol. 2001;45:487–498.
13. Tanew A, Guggenbichler A, Honigsmann H, et al. Photochemotherapy for severe psoriasis without or in combination with acitretin: a randomized, double-blind comparison study. J Am Acad Dermatol. 1991;25:682–684.
14. Lebwohl M, Christopers E, Langley R, et al. An international, randomized, double-blind, placebo-controlled phase 3 trial of intramuscular alefacept in patients with chronic plaque psoriasis. Arch Dermatol. 2003;139:719–727.
15. Soriatane [package insert]. Palo Alto, Calif: Connetics; 2004
16. Heydendael VM, Spuls PI, Opmeer BC, et al. Methotrexate versus cyclosporine in moderate-to-severe chronic plaque psoriasis. N Engl J Med. 2003;349:658–665.
17. AHFS First Web. AHFS Drug Information Handbook online. Cyclosporine and methotrexate monographs. San Bruno, Calif: First Databank Incorporated; 2002. Accessed May 19, 2005.
18. Naldi L, Griffiths CE. Traditional therapies in the management of moderate to severe chronic plaque psoriasis: an assessment of the benefits and risks. Br J Dermatol. 2005;152(4):597–615.
19. Feldman SR. Topics in Psoriasis. Medscape Today, 2003. Available at: http:// http://www.medscape.com/viewarticle/453360. Accessed May 27, 2005.
20. Amevive [package insert]. Cambridge, Mass: Biogen Idec; 2004.
21. Gordon KB, Vaishnaw AK, O'Gorman J, et al. Treatment of psoriasis with alefacept. Correlation of clinical improvement with reductions of memory T-cell counts. Arch Dermatol. 2003; 139:1563–1570.
22. Lowe NJ, Gonzalez J, Bagel J, et al. Repeat courses of intravenous alefacept in patients with chronic plaque psoriasis provide consistent safety and efficacy. Inter Soc Dermatol. 2003;42:224–230.
23. Krueger GG. Clinical response to alefacept: results of a phase 3 study of intravenous administration of alefacept in patients with chronic plaque psoriasis. J Europ Acad DermatolVenereol. 2003;17(suppl 2):17-24.
24. Gordon KB, Langley RG. Remittive effects of intramuscular alefacept in psoriasis. J Drugs Dermatol. 2003;2:624–628.
25. Ortonne JP, Lebwohl M, Griffiths CEM. Alefacept-induced decreases in circulating blood lymphocyte counts correlate with clinical response in patients with chronic plaque psoriasis. Eur J Dermatol. 2003;13:117–123.
26. Raptiva [package insert]. South San Francisco, Calif: Genentech Inc; 2004.
27. Gordon KB, Papp KA, Hamilton TK, et al. Efalizumab for patients with moderate to severe plaque psoriasis. A randomized controlled trial. JAMA. 2003;290:3073–3080.
28. FDA Center for Drug Evaluation and Research. Food and Drug Administration website. Available at: http:// http://www.fda.gov/ohrms/dockets/ac/03/briefing/3983±_02_fda-raptiva.pdf. Accessed May 27, 2005.
29. Lebwohl M, Tyring SK, Hamilton TK, et al. A novel targeted T-cell modulator, efalizumab, for plaque psoriasis. New Engl J Med. 2003; 21:2004–2013.
30. Menter A, Gordon K, Carey W, et al. Efficacy and safety observed during 24 weeks of efalizumab therapy in patients with moderate to severe plaque psoriasis. Arch Dermatol. 2005;141:31–38.
31. Leonardi C, Papp K, Gordon K, et al. Extended efalizumab therapy improves chronic plaque psoriasis: results from a randomized phase III trial.J Am Acad Dermatol. 2005;52:425–433.
32. Gottlieb A, Gordon K, Hamilton T, et al. Maintenance of efficacy and safety with continuous efalizumab therapy in patients with moderate to severe chronic plaque psoriasis: final phase IIIb study results [abstract]. Presented at: the American Academy of Dermatology Annual Meeting; February 18–22, 2005; New Orleans, La. Abstract P4.
33. Humira [package insert]. Abbott Park, Ill: Abbott Laboratories; 2004.
34. Chen D, Gordon K, Leonardi C, Menter A. Adalimumab efficacy and safety in patients with moderate to severe chronic plaque psoriasis: preliminary findings from a 12-week dose-ranging trial [abstract]. Presented at: the American Academy of Dermatology Annual Meeting; February 6–11, 2004; Washington, DC. Abstract P2.
35. Langley R, Leonardi C, Toth D, et al. Long term safety and efficacy of adalimumab in the treatment of moderate to severe chronic plaque psoriasis [abstract]. Presented at: the American Academy of Dermatology Annual Meeting; February 18–22, 2005; New Orleans, La. Abstract P8.
36. Remicade [package insert]. Malvern, Penn: Centocor Inc; 2005.
37. Keane J, Gershon SK, Braun MM. Tuberculosis and treatment with infliximab. N Engl J Med. 2002;346:625–626.
38. Gottlieb AB, Evans R, Menter A: Infliximab in the Treatment of Psoriasis: Results from the first 10 weeks of the phase II trial [abstract]. Presented at: the American Academy of Dermatology Annual Meeting; March 21–26, 2003; San Francisco, Calif. Abstract P596.
39. Chaudhari U, Romano P, Mulcahy LD, et al. Efficacy and safety of infliximab monotherapy for plaque-type psoriasis: a randomised trial. Lancet. 2001;357:1842–1847.
40. Gottlieb AB, Chaudhari U, Mulcahy LD, et al. Infliximab monotherapy provides rapid and sustained benefit for plaque-type psoriasis. J Am Acad Dermatol. 2003;48:829–835.
41. Enbrel [package insert]. Thousand Oaks, Calif: Immunex Corp; 2004.
42. Louie SG, Park B, Yoon H. Biological response modifiers in the management of rheumatoid arthritis. Am J Health Syst Pharm. 2003;60: 346–355.
43. Mikuls TR, Moreland LW. TNF blockade in the treatment of rheumatoid arthritis: infliximab versus etanercept. Expert Opin Pharmacother. 2001;2:75–84.
44. Gottlieb AB, Matheson RT, Lowe N, et al. A randomized trial of etanercept as monotherapy for psoriasis. Arch Dermatol. 2003;139:1627–1632.
45. Leonardi CL, Powers JL, Matheson RT, et al. Etanercept as monotherapy in patients with psoriasis. New Engl J Med. 2003;349:2014–2022.
46. FDA Center for Drug Evaluation and Research. Efalizumab Medical Review, Part 1. Available at: http:// http://www.fda.gov/cder/foi/nda/2003/125075_0000_Raptiva_Medr_P1.pdf. Accessed May 27, 2005.
47. The National Psoriasis Foundation website. Available at: http:// http://www.psoriasis.org/research/pipeline/chart.php. Accessed May 27, 2005.
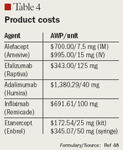
48. Drug Topics Red Book (update). July 2004 and May 2005.
49. Wanke LA, Chiou CF, Woolley M. Cost efficacy comparison of biologics in the treatment of psoriasis [abstract]. Presented at: the American Academy of Dermatology Annual Meeting; February 6–11, 2004; Washington, DC. Abstract P699.
50. Feldman SR, Garton R, Averett W, et al. Strategy to manage the treatment of severe psoriasis: considerations of efficacy, safety, and cost. Expert Opin Pharmacother. 2003;4:1525–33.
51. Abramovits W, Stevenson L. Comparison of biologic therapies for the treatment of psoriasis. Presented at the American Academy of Dermatology Annual Meeting, February 18–22, 2005; New Orleans LA. Poster P2.
Scripius Removes Dupixent from Formulary
September 7th 2023The decision by Scripius (previously Select Health Prescriptions) was made based on the cost of Dupixent, as well as because of an increased demand to use Dupixent for mild atopic dermatitis when the primary patient population is those with moderate to severe disease.
