- Safety & Recalls
- Regulatory Updates
- Drug Coverage
- COPD
- Cardiovascular
- Obstetrics-Gynecology & Women's Health
- Ophthalmology
- Clinical Pharmacology
- Pediatrics
- Urology
- Pharmacy
- Idiopathic Pulmonary Fibrosis
- Diabetes and Endocrinology
- Allergy, Immunology, and ENT
- Musculoskeletal/Rheumatology
- Respiratory
- Psychiatry and Behavioral Health
- Dermatology
- Oncology
Eslicarbazepine: A novel antiepileptic agent designed for improved efficacy and safety
Eslicarbazepine acetate (eslicarbazepine, or ESL) is a new antiepileptic agent awaiting FDA approval.

Key Points
Abstract
The International League Against Epilepsy classify epilepsy into 3 main types: partial, generalized, and unclassified. Partial epilepsy is restricted to discrete areas of the cerebral cortex while generalized epilepsy occurs in diffuse regions of the brain simultaneously. Treatment of partial-onset seizures presents a constant challenge since up to 58% of patients with partial-onset seizures do not achieve seizure control with current antiepileptic drugs. Patient compliance with antiepileptic agents represents a significant area of unmet need, with poorly compliant patients more likely to experience breakthrough seizures and mortality. Finally, adverse events, such as dizziness and somnolence, are highly prevalent with existing antiepileptic agents and may affect as many as 97% of patients. Eslicarbazepine acetate (eslicarbazepine, or ESL) is a novel antiepileptic agent, a derivative of carbamazepine and oxcarbazepine, designed for improved efficacy and safety. In clinical trials, ESL demonstrated efficacy and was generally well tolerated. It also demonstrated low potential for drug-drug interaction. A New Drug Application for ESL for adjunctive therapy in adults with partial-onset seizures was accepted by FDA for formal review in June 2009 and FDA is expected to act on the application by January 2010. (Formulary. 2009;44:357-361.)
Epilepsy is one of the most common neurological diseases affecting more than 3 million people in the United States.1
Eslicarbazepine acetate (eslicarbazepine, or ESL) is a novel antiepileptic agent designed for improved efficacy and safety. It is a derivative of carbamazepine, oxcarbazepine, and a prodrug of the main active metabolite (S)-licarbazepine (one of the enantiomers of the monohydroxy derivative of oxcarbazepine).9 A New Drug Application (NDA) for ESL (Stedesa, Sepracor) was filed by the manufacturer in March 2009 for adjunctive therapy in the treatment of partial-onset seizures in adults with epilepsy and FDA accepted the filing for formal review in June 2009. The Prescription Drug User Fee Act (PDUFA) action date (date by which FDA is expected to review and act on an NDA submission) for Stedesa is January 30, 2010.10
ESL [(S)-(-)-10-acetoxy-10,11-dihydro-5H-dibenz[b,f]azepine-5-carboxamide], is a novel central nervous system (CNS)-active compound with anticonvulsant activity. It acts as a voltage-gated sodium channel (VGSC) blocker and inhibits sodium-channel dependent release of neurotransmitter with potency similar to carbamazepine and oxcarbazepine. ESL competitively interacts with "site 2" of the inactivated state of voltage-gated sodium channels, stabilizes the inactive form of the sodium channel, and sustains repetitive neuronal firing. A modification at the 10,11-position results in a metabolism that does not undergo auto-induction.11
PHARMACOKINETICS
ESL is rapidly and extensively metabolized in the liver to the major metabolite S-licarbazepine by liver esterases. Minor metabolites of ESL are (R)-licarbazepine and oxcarbazepine. Approximately 95% of ESL appears in plasma as (S)-licarbazepine with only 5% converted to (R)-licarbazepine.12 Approximately 30% of ESL binds to plasma proteins, and time to maximum concentration is attained 1 to 4 hours post dose.13
The half life of ESL after single-dose application is 8 to 17 hours, but with repeated application, the half-life is 20 to 24 hours.14,15 ESL pharmacokinetics in healthy adults are not significantly affected by age or gender.14
ESL is excreted primarily by renal excretion. A study in patients with mild to severe renal impairment showed that renal clearance of ESL changes with creatinine clearance and thus dose adjustment is required in the presence of renal failure.
Data support the use of half the dose in patients with ClCr 30 to 60 mL/min but dosing in patients with CrCl <30 mL/min has not been clearly determined.
In patients with end stage renal disease, dialysis is effective at removing ESL metabolites from plasma.15 No dose adjustment is necessary in patients with moderate hepatic impairment.
CLINICAL TRIALS
The effectiveness of ESL as an adjunctive treatment in adults with refractory partial-onset seizures was evaluated in four randomized, double-blind, placebo-controlled, multinational, 12-week trials.16,17,18,19 The trials included a fully-published phase 2 dose frequency comparison (n=143)16 and three phase 3, once-daily dosage comparisons (BIA-2093-301 [n=402] fully published, BIA-2093-302 [n=393] and BIA-2093-303 [n=252], only available as posters).17,18,19 Each were identified by the investigational drug name BIA-2093. In all phase 3 trials, patients completing the double-blind treatment period were eligible to receive ESL in open-label, 1-year extension studies. Data on long-term efficacy in the extension to study BIA-2093-302 are available as a poster.20
All studies were conducted in men or women ≥18 years, who experienced simple or complex partial seizures with or without secondary generalization for ≥12 months, and were experiencing at least 4 partial-onset seizures per month despite treatment with 1 to 2 or 1 to 3 AEDs in stable doses for at least 2 months with no seizure-free interval for >21 consecutive days. A majority of patients were taking 2 AEDs at baseline and were continued on it throughout the trials. In the phase 2 trial, patients were excluded if they had received carbamazepine or oxcarbazepine in the previous 6 months.
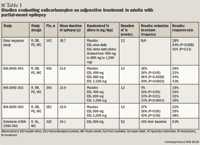
BIA-2093-301 trial (2009)17 was a phase 3 trial that assessed the efficacy and safety of ESL as adjunctive therapy for refractory partial seizures in adult patients. Patients were randomly assigned to 1 of 4 groups: placebo (n=100), ESL 400 mg once daily (n=100), ESL 800 mg once daily (n=98), or ESL 1,200 mg once daily (n=102). The daily dose was titrated weekly by 400 mg to reach the maintenance dose. The mean age of patients was approximately 39 years, 51% were women and all patients were Caucasians. Most patients (82%) completed the trial. The primary end point was the least square mean seizure frequency adjusted per 4 weeks from an analysis of covariance of log transformed seizure frequency in the ITT population. Seizure frequency was significantly lower than placebo in the ESL 1,200 mg and ESL 800 mg groups as compared to the placebo group. The most frequent concomitant AEDs were carbamazepine, lamotrigine, and valproic acid. Results were similar in patients administered ESL with or without carbamazepine as concomitant AED. BIA-2093-302 trial18 was the second phase 3 trial that assessed the efficacy and safety of ESL as adjunctive therapy for refractory partial seizures in adult patients. Patients were randomly assigned to 1 of 4 groups: placebo (n=100), ESL 400 mg once daily (n=96), ESL 800 mg once daily (n=100), or ESL 1,200 mg once daily (n=97). Patients in the ESL 1,200 mg group received 800 mg in the first 2-week titration period. The other groups had no titration scheme and started the maintenance dose in the 2 weeks before the maintenance period. The median age of patients was 35 years and 51% were women while 88% were Caucasians. A majority of patients (>70%) were taking 2 AEDs and most patients (82%) completed the trial.
The primary end point was the least square mean seizure frequency adjusted per 4 weeks from an analysis of covariance of log transformed seizure frequency in the ITT population. Seizure frequency over the maintenance period was significantly lower than placebo in the ESL 1,200 mg and ESL 800 mg groups. The most frequent concomitant AEDs were carbamazepine (60%), valproic acid (22%), and lamotrigine (21%).
BIA-2093-303 trial19 was the final phase 3 trial that assessed the efficacy and safety of ESL as adjunctive therapy for refractory partial seizures in adult patients.
Patients were randomly assigned to 1 of 3 groups: placebo (n=87), ESL 800 mg once daily (n=85), or ESL 1,200 mg once daily (n=80). Patients were given half of the maintenance dose during the 2-week titration period. Patients who completed the maintenance period entered a 4-week tapering-off period, during which the ESL dose was decreased to a half for the first 2 weeks, and received placebo for the following 2 weeks. The median age of patients was 35 years and 55% were women while 38% were Caucasians. A majority of patients (>75%) were taking 2 AEDs and most patients (77%) completed the trial. The primary end point was the least square mean seizure frequency adjusted per 4 weeks from an analysis of covariance of log transformed seizure frequency in the ITT population. Seizure frequency over the maintenance period was significantly lower than placebo in the ESL 800 mg and ESL 1,200 mg groups. The most frequent concomitant AEDs were carbamazepine (56%), valproic acid (31%), and levetiracetam (21%).
OPEN-LABEL EXTENSION
Patients completing the double-blind, placebo-controlled BIA-2093-302 study and entering the open-label extension study received ESL 800 mg once daily for the first 4 weeks, after which dosages were titrated up or down in 400 mg steps according to clinical response.20 Of 325 patients enrolled in the extension study (94 of whom received placebo in the double-blind study), 267 patients received ESL for 6 months and 223 for 1 year. The mean dosage of ESL over the 1-year period was 877 mg once daily. The most common concomitant AEDs were carbamazepine, valproic acid, lamotrigine, topiramate, levetiracetam, Phenobarbital, and clonazepam.
Overall, 204 patients received two concomitant AEDs, 107 received 1 AED, and 2 patients received 3 AEDs. Relative to baseline values from the double-blind trial, the mean relative reductions in seizure frequency per period in the ITT population were 32%, 38%, and 41% for weeks 1 to 4, 5 to 16, and 41 to 52, respectively. The responder rates were 41% for weeks 1 to 4 and 53% for weeks 41 to 52. The proportion of seizure-free patients per 12-week period increased from 8.7% at weeks 5 to 16 to 12.5% at weeks 41 to 52.
ADVERSE EFFECTS
The safety of ESL was evaluated in the clinical trials discussed above.16-19 Treatment emergent adverse events were reported by 38% to 80% of ESL recipients compared with 31% to 45% of placebo recipients in phase 2/3 clinical trials. The number of adverse events generally increased with dosage and most were of mild to moderate severity. Severe adverse events were reported in 0% to 6% of ESL recipients compared with 0% to 4% of placebo recipients.16-19 Discontinuation rates as a result of treatment-emergent adverse events increased with ESL in phase 3 trials, being 4% to 13% for the 400 mg/day groups, 8% to 19% for the 800 mg/day groups, and 11% to 27% for the 1,200 mg/day groups.17-19 There were no treatment-related deaths.16-20 The most common treatment-emergent adverse events, defined as adverse events with an incidence >10% in ESL recipients in phase 3 clinical trials, were dizziness, somnolence, headache, nausea, diplopia, abnormal coordination, and vomiting.17-19 Most of the adverse events occurred early in the treatment with 48% occurring in the titration period and another 33% in the first 4 weeks of maintenance therapy in one study.18 In the 1-year, open-label extension of study BIA-2093-302, 83% of patients experienced, at least once, a treatment-emergent adverse event, of which 82% were of mild to moderate severity.20 The most common adverse events were dizziness (27%), headache (16%), somnolence (12%), abnormal coordination (9%), hypotension (9%), and diplopia (9%), vomiting (7%), nausea (7%), nasopharyngitis (6%), diarrhea (5%), back pain (5%), and blurred vision (5%). Overall, 11% of patients discontinued therapy as a results of adverse events.20
DRUG INTERACTIONS
ESL has no effect on the activity of numerous cytochrome P450 isoenzymes, uridine diphosphate glucuronyltransferase-glucuronosyltransferase and epoxide hydrolases in human microsomes. It does not affect plasma concentrations of carbamazepine, lamotrigine, levetiracetam, topiramate, phenobarbital, or diazepam.17 ESL 1,200 mg daily given concomitantly with a hormonal oral contraceptive containing 30 mcg ethinyl estradiol and 150 mcg levonorgestrel was shown to decrease the plasma concentrations of the 2 hormonal components when compared against oral contraceptive alone.11 ESL at a daily dose of 1,200 mg produced a mild but significant decrease in S-warfarin concentrations, but with no impact on INR levels.11 ESL 1,200 mg daily did not have an effect on digoxin pharmacokinetics in healthy individuals. In vitro studies showed that the binding of ESL to plasma protein is relatively low and is not affected by the presence of warfarin, diazepam, digoxin, phenytoin, and tolbutamide.11
DOSING
Although there are no formal dosage and administration recommendations for ESL in the treatment of epilepsy, oral dosages of 800 mg and 1,200 mg once daily have been shown to be effective in the adjunctive treatment of adults experiencing partial-onset seizures in phase 3 clinical trials.17-19 In a long-term extension of phase 3 trial, the median dosage of ESL on which patients were stabilized was 800 mg once daily.20 Planned commercialization of ESL appears to be in the form of the 800 mg and 1,200 mg tablets.
FORMULARY CONSIDERATIONS
Treatment of partial-onset seizures presents a constant challenge because up to 58% of patients with partial-onset seizures do not achieve seizure control with current AEDs.5 Adverse events, such as dizziness and somnolence, are highly prevalent with existing antiepileptic agents and may affect as many as 97% of patients.8
ESL is a novel derivative of carbazepine and oxcarbazepine designed for improved efficacy and safety in adjunctive treatment of adults with partial-onset epilepsy.11 ESL is designed for once-daily administration which can lead to enhanced patient compliance compared to other AEDs that required multiple daily dosing. It also has the potential to offer additional seizure control with a simpler dosage titration schedule.17-19
In clinical trials evaluating ESL's efficacy in patients with partial-onset seizures, ESL at doses of 800 mg and 1,200 mg demonstrated statistically significant reductions in seizure frequency compared to placebo.17-19 It also improved the response rate compared to placebo. The pharmacokinetic and pharmacodynamic profiles show non-significant interactions with other AEDs which makes it more desirable compared to other AEDs that have significant drug-drug interactions.17
ESL does reduce the effectiveness of oral contraceptives and caution is warranted. Since ESL is predominantly renally eliminated, its use with AEDs that induce or inhibit liver enzymes is not expected to affect ESL's serum concentration and no dosage adjustment is necessary for patients who have moderate hepatic impairment.15 Conversely, dose adjustment is required in renal impairment and the dosing in renal dysfunction is not yet known.
The available studies demonstrate that ESL is well tolerated and effective when used as adjunctive therapy for adult patients with refractory partial-onset epilepsy.
Although clinical trials of modest size with relatively short follow-up periods are not the best study design to evaluate long-term safety, the trial results and the results of the 1-year extension of a phase 3 trial suggest a favorable safety profile.20 Common adverse events occurring more frequently with ESL group compared to placebo include dizziness, somnolence, headache, nausea, diplopia, abnormal coordination, and vomiting.17-19
ESL offers several advantages over current AEDs in market. However, cost of ESL is not yet known and may prove to be more expensive compared to other AEDs. Studies are currently evaluating the possible role of ESL in children and adolescents.21
Ultimately, the results from ongoing studies and further clinical experience will dictate the clinical utility of this agent, if approved. The manufacturer, Sepracor, has submitted an NDA which was accepted for review by the FDA in June 2009 and by January 2010, FDA is expected to review and act on the submission.
Dr Talati is research scientist, Hartford Hospital, Hartford, CT; Dr White is associate professor of pharmacy and director of the University of Connecticut, Hartford Hospital Evidence-based Practice Center, Hartford; Dr Coleman is associate professor of pharmacy practice, University of Connecticut School of Pharmacy, and director, Pharmacoeconmics and Outcomes Studies Group, Hartford Hospital, Storrs, CT.
Disclosure Information: The authors report no financial disclosures as related to products discussed in this article.
In each issue, the "Focus on" feature reviews a newly approved or investigational drug of interest to pharmacy and therapeutics committee members. The column is coordinated by Robert A. Quercia, MS, RPh, clinical manager, Department of Pharmacy Services, Hartford Hospital, Hartford, Conn, and adjunct associate professor, University of Connecticut School of Pharmacy, Storrs, Conn; and by Craig I. Coleman, PharmD, associate professor of pharmacy practice, University of Connecticut School of Pharmacy, and director, Pharmacoeconomics and Outcomes Studies Group, Hartford Hospital.
EDITORS' NOTE: The clinical information provided in "Focus on" articles is as current as possible. Due to regularly emerging data on developmental or newly approved drug therapies, articles include information published or presented and available to the author up until the time of the manuscript submission.
REFERENCES
1. The Epilepsy Foundation of America. Available at: http://www.epilepsyfoundation.org/about/statistics.cfm. Accessed August 28, 2009.
2. Tatum IV WO, Benbadis SR, Vale FL The neurosurgical treatment of epilepsy. Arch Fam Med. 2000;9:1142-1146.
3. Middleton DB. Seizure disorders. In: Taylor RB ed. Family Medicine: Principles and Practice. 6th ed. New York, NY: Springer-Verlag;2003, chap 64.
4. Lowenstein DH. Seizures and Epilepsy. In: Fauci AS, Kasper DL, Longo DL eds. Harrison's Principles of Internal Medicine. 17th ed. New York, NY: McGraw-Hill;2008, chap 363.
5. Brodie MJ. Management strategies for refractory localization-related seizures. Epilepsia. 2001;42(suppl 3):27-30.
6. Cramer JA, Glassman M, Rienzi V. The relationship between poor medication compliance and seizures. Epilepsy Behav. 2002;3:338-342.
7. Faught E, Duh M, Weiner J, Guérin A, Cunnington M. Nonadherence to antiepileptic drugs and increased mortality: Findings from the RANSOM study. Neurology. 2008;71:1572-1578.
8. Mei PA, Montenegro MA, Guerreiro MM, Guerreiro CA. Pharmacovigilance in epileptic patients using antiepileptic drugs. Arg Neuropsiquiatr. 2006;64:198-201.
9. Johannessen Landmark C, Johannessen SI. Pharmacological management of epilepsy: recent advances and future prospects. Drugs. 2008;68(14):1925-39.
10. Sepracor's STEDESA (Eslicarbazepine Acetate) New Drug Application Formally Accepted for Review by the FDA. Available at: http://www.istockanalyst.com/article/viewiStockNews/articleid/3306440/. Accessed September 24, 2009.
11. Almeida L, Soares-da-Silva P. Eslicarbazepine acetate (BIA-2-093). Neurotherapeutics. 2007;4:88-96.
12. Maia J, Vaz-da-Silva M, Almeida L, et al. Effect of food on the pharmacokinetic profile of eslicarbazepine acetate (BIA 2-093). Drugs. 2005;6:201-206.
13. Bialer M, Johannessen SI, Kupferberg HJ, Levy RH, Perucca E, Tomson T. Progress report on new antiepileptic drugs: a summary of the Eighth Eilat Conference (EILAT VIII). Epilepsy Res. 2007;73:1-52.
14. Almeida L, Falcão A, Maia J, Mazur D, Gellert M, Soares-da-Silva P. Single-dose and steady-state pharmacokinetics of eslicarbazepine acetate (BIA 2-093) in healthy elderly and young subjects. J Clin Pharmacol. 2005;45:1062-1066.
15. Maia J, Almeida L, Falcão A, et al. Effect of renal impairment on the pharmacokinetics of eslicarbazepine acetate. Int J Clin Pharmacol Ther. 2008;46:119-130.
16. Elger C, Bialer M, Cramer JA, Maia J, Almeida L, Soares-da-Silva P. Eslicarbazepine acetate: a double-blind, add-on, placebo-controlled exploratory trial in adult patients with partial-onset seizures. Epilepsia. 2007;48(3):497-504.
17. Elger C, Halász P, Maia J, Almeida L, Soares-da-Silva P. Efficacy and safety of eslicarbazepine acetate as adjunctive treatment in adults with refractory partial-onset seizures: a randomized, double-blind, placebo-controlled, parallel-group phase III study. Epilepsia. 2009;50(3):454-463.
18. Ben-Menachem E, Gabbai AA, Hufnagel A, Maia J, Almeida L, Soares-da-Silva P. Efficacy and safety of eslicarbazepine acetate (ESL) as add-on treatment in adults with refractory partial-onset seizures. BIA-2093-302 study. Poster presented at the American Epilepsy Society (AES) 62nd Annual Meeting, Seattle, Washington, December 8, 2008.
19. Gil-Nagel A, Lopes-Lima J, Maia J, Almeida L, Soares-da-Silva P. Efficacy and safety of eslicarbazepine acetate (ESL) as add-on treatment in adults with refractory partial-onset seizures: BIA-2093-303 study. Poster presented at the American Epilepsy Society (AES) 62nd Annual Meeting, Seattle, Washington, December 8, 2008.
20. Gabbai AA, Ben-Menachem E, Maia J, Almeida L, Soares-da-Silva P. Long-term treatment of partial epilepsy with eslicarbazepine acetate (ESL): results of a one-year open-label extension of study BIA-2093-302. Poster presented at the American Epilepsy Society (AES) 62nd Annual Meeting, Seattle, Washington, December 8, 2008.
21. Almeida L, Minciu I, Nunes T, et al. Pharmacokinetics, efficacy, and tolerability of eslicarbazepine acetate in children and adolescents with epilepsy. JClin Pharmacol. 2008;48:966-977.
Employers Face Barriers With Adopting Biosimilars
March 1st 2022Despite the promise of savings billions of dollars in the United States, adoption of biosimilars has been slow. A roundtable discussion among employers highlighted some of the barriers, including formulary design and drug pricing and rebates.
