- Safety & Recalls
- Regulatory Updates
- Drug Coverage
- COPD
- Cardiovascular
- Obstetrics-Gynecology & Women's Health
- Ophthalmology
- Clinical Pharmacology
- Pediatrics
- Urology
- Pharmacy
- Idiopathic Pulmonary Fibrosis
- Diabetes and Endocrinology
- Allergy, Immunology, and ENT
- Musculoskeletal/Rheumatology
- Respiratory
- Psychiatry and Behavioral Health
- Dermatology
- Oncology
Health Plans Release 2024 Prescription Changes in Medicare Plans
Aetna, Cigna, Humana, United Healthcare — some of the largest providers of Medicare Advantage plans — have released updates to prescription drug programs.
Medicare enrollment has been steadily increasing. As of March 2023, 65.7 million people are enrolled in Medicare, an increase of almost 100,000 since the last report in September. Of these, 51.6 million are enrolled in Medicare Part D in stand-alone prescription drug plans, as well as Medicare Advantage plans that offer prescription drug coverage.
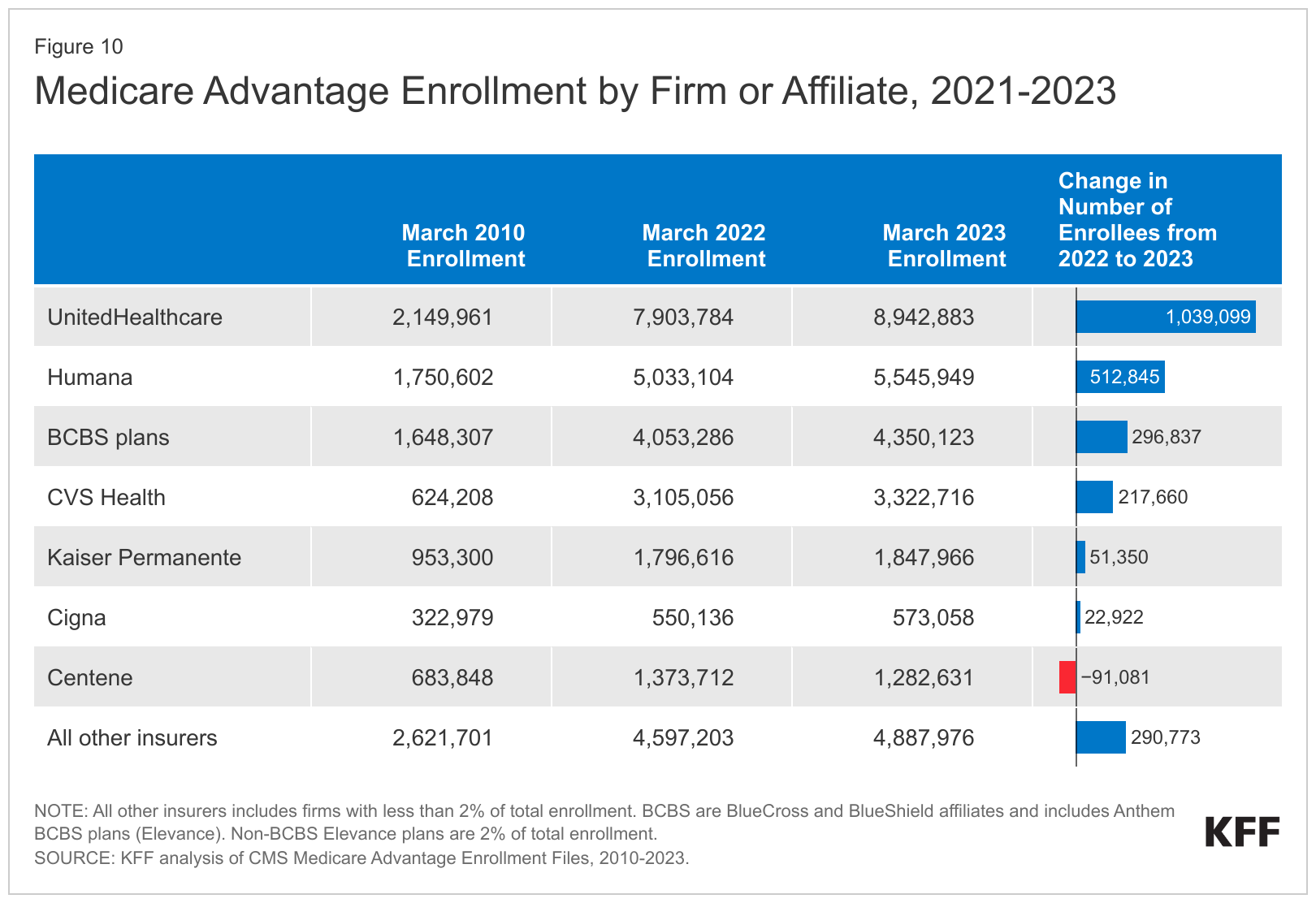
And enrollment in Medicare Advantage Plans has also been increasing, growing by 2.3 million beneficiaries from 2022 to 2023. In 2023, 30.8 million people are enrolled in a Medicare Advantage plan, accounting for more than half, or 51%, of the eligible Medicare population. UnitedHealthcare and Humana account for nearly half (47%) of all Medicare Advantage enrollees nationwide, according to an analysis in August by KFF. Four additional firms — CVS Health, Kaiser Permanente, Centene, and Cigna — account for another 23% of enrollment in 2022. (See Table below)
For 2024, health plans have made some changes and update to their plan and prescriptions offerings. Many have expanded the formularies with additional drugs available at $0 copay on certain drugs in the lower tiers. Some have additional drugs to the formularies and to dual eligible and special needs plans.
Open enrollment for Medicare plans begins Oct. 15, 2023. Medicare annual enrollment runs through Dec. 7, 2023, with coverage beginning in January 2024. Below is a look at some of the prescription drug changes for 2024.
Aetna (CVS)
In 2024, Aetna, a CVS Healthcare company, has strengthened its core benefits, offering $0 copays for tier 1 drugs and an OTC allowance, the company said in a press release. In addition, Aetna’s Medicare Advantage dual eligible special needs plans (D-SNPs), designed for individuals who are eligible for both Medicare and Medicaid, has an expanded network of participating retailers for the Aetna Medicare Extra Benefits card. The program is a debit card that can be used to purchase certain items, include nonprescription drugs, healthy foods, personal care items and transportation.
In addition, qualifying members can receive a quarterly allowance on the Aetna Medicare Payment Card to use toward either out-of-pocket expenses for in-network care or select OTC wellness items at any CVS Pharmacies or place orders online through OTC Health Solutions, a CVS Health company.
In the stand-alone Medicare Advantage Prescription Drug Plans, Aetna has several made several changes, including:
- All members have $0 deductible on all tier 1 and tier 2 drugs. Some plans have a $0 deductible on all tiered drugs.
- $0 copays at preferred network pharmacies on tier 1 drugs. Some plans have $0 copays on tier 1 and tier 2 drugs for 30-, 60- or 100-day supplies.
- $35 for a one-month supply of each insulin product covered by the plan.
- Many covered Part D vaccines will be available at $0 copay for Medicare beneficiaries.
- Up to a 100-day supply for drugs on tiers 1–4 at both retail and mail-order pharmacies with no-cost standard shipping.
Cigna
Cigna is offering three stand-alone Prescription Drug Plans in all 50 states, the District of Columbia and Puerto Rico. All plans have $0 copay options for select medications purchased through preferred home delivery. The three plans include: Cigna Saver Rx, Cigna Secure Rx, and Cigna Extra Rx. But a press release from the company didn’t offer any specific changes in its prescription drug programs, and the company has not responded to a request for more information.
Humana
In 2024, Humana is offering preferred mail order prescriptions with $0 tier 1 and tier 2 prescriptions for a three-month supply in all plans. Humana members have the option to use CenterWell Pharmacy, a home delivery pharmacy, the company said in a press release. All of Humana’s Medicare
Humana updated its stand-alone Prescription Drug Plans. Its generic focused plan, the Humana Walmart Value Rx plan, offers $0 tier 1 and tier 2 copays at preferred pharmacies and a $0 deductible on tier 1 and tier 2 drugs. Humana Premier Rx plan will offer a new $0 tier 6 for some drugs at preferred pharmacies; tier 1, tier 2 and tier 6 medications include a $0 deductible and additional gap coverage. Additionally, Humana is offering $0 copays for 90-day supplies of tier 1 and 2 medications at CenterWell Pharmacy
United Health
In 2024, patients in UnitedHealthcare’s Medicare Advantage plans will see stable copays for prescription drugs. The health plan has released 2024 updates to its drug coverage in Medicare Advantages, and company executives said in a press release that it will now cover more of the most-used tier 1 prescriptions than any national competitor.
Some of the updates include:
- The Medicare Advantage formulary will cover more of the most-used tier 1 prescriptions
- A month supply of insulin is $35 for standard plans.
- Tier 2 coverage will be expanded to include four commonly used non-Medicare covered drugs (generic Viagra, folic acid, vitamin D, B12).
- All members will have $0 tier 1 and tier 2 copays with Optum Home Delivery.
In Medicare Advantage plans for patients with chronic disease special needs (C-SNP), members will pay a $25 or less copay for covered insulin. UnitedHealthcare said that enrollment in C-SNP plans could save members with diabetes could save up to $50 each month on diabetic supplies and insulin compared with the standard UnitedHealthcare Medicare Advantage plan. Additionally, 23 prescriptions commonly used to treat conditions required for enrollment are on lower-cost tiers in the C-SNP plan than the standard formulary.
Medicare Advantage dual eligible special needs plans (D-SNPs) include $0 copays all year long on all covered Part D prescriptions, as well as a Healthy Options Allowance with rollover.
Source: KFF