- Safety & Recalls
- Regulatory Updates
- Drug Coverage
- COPD
- Cardiovascular
- Obstetrics-Gynecology & Women's Health
- Ophthalmology
- Clinical Pharmacology
- Pediatrics
- Urology
- Pharmacy
- Idiopathic Pulmonary Fibrosis
- Diabetes and Endocrinology
- Allergy, Immunology, and ENT
- Musculoskeletal/Rheumatology
- Respiratory
- Psychiatry and Behavioral Health
- Dermatology
- Oncology
Non-elderly patients with overactive bladder have significant comorbidities
A study was conducted to evaluate the clinical and economic burden of overactive bladder (OAB) among patients <60 years of age in a managed care population, especially with regard to the prevalence of related comorbidities and associated annual medical costs.
A study was conducted to evaluate the clinical and economic burden of overactive bladder (OAB) among patients <60 years of age in a managed care population, especially with regard to the prevalence of related comorbidities and associated annual medical costs.
INTRODUCTION
An estimated 33.3 million adults in the United States suffer from OAB with an associated cost of more than $12 billion annually.1,2 The additional costs related to treating OAB comorbidities such as falls and fractures, depression, urinary tract infections (UTIs), skin infections, and vulvovaginitis are substantial.3 OAB is often considered a condition of the elderly and few studies have examined the clinical and economic impact of the condition in younger individuals.4–10
Patients with OAB between the ages of 18 and 59 years during January 1 through June 30, 2002, were identified through a retrospective analysis of healthcare claims data of 2.7 million members from a US managed care organization and were followed for 1 year.
A random sample of controls without OAB was matched 1:1 to the study group on demographics and on relevant clinical conditions using propensity score matching.
The primary outcome measure was the proportion of patients with a primary or secondary diagnosis of the following comorbidities: falls and fractures, depression, UTIs, skin infections, and vulvovaginitis. The likelihood of these comorbidities in the OAB versus control group was calculated as odds ratios.
Logistic regression was used to compare OAB patients with controls, adjusting for additional clinical characteristics such as neurologic conditions, diuretic use, inappropriate use of select medications from the Beers criteria,11 prostatic hyperplasia, and bladder neoplasm that could increase the likelihood of studied comorbidities.
Mean annual submitted medical charges were calculated for each comorbidity among the subset of members who incurred medical charges for that condition.
RESULTS
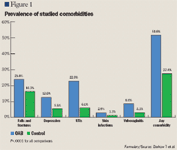
Patients with OAB were significantly more likely than controls to have each of the studied comorbidities after adjustment for contributing factors. The odds ratios of patients with OAB having the comorbidities compared with controls (P<.0001 for all comparisons) were: UTIs, 4.7; vulvovaginitis, 2.9; depression, 2.5; skin infections, 2.2; and falls and fractures, 1.6. Overall, patients with OAB were 2.8 times more likely (P<.0001) to have at least 1 of these comorbid conditions compared with controls.
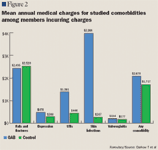
Discussion

Employers Face Barriers With Adopting Biosimilars
March 1st 2022Despite the promise of savings billions of dollars in the United States, adoption of biosimilars has been slow. A roundtable discussion among employers highlighted some of the barriers, including formulary design and drug pricing and rebates.
