- Safety & Recalls
- Regulatory Updates
- Drug Coverage
- COPD
- Cardiovascular
- Obstetrics-Gynecology & Women's Health
- Ophthalmology
- Clinical Pharmacology
- Pediatrics
- Urology
- Pharmacy
- Idiopathic Pulmonary Fibrosis
- Diabetes and Endocrinology
- Allergy, Immunology, and ENT
- Musculoskeletal/Rheumatology
- Respiratory
- Psychiatry and Behavioral Health
- Dermatology
- Oncology
P&T considerations in fashioning a knowledge base, action plan for cardiometabolic disorders and weight
The P&T committee is positioned to provide knowledge, strategies to improve treatment of patients with cardiometabolic disorders.

Key Points
Abstract
Almost 25% of US adults have a constellation of abnormalities constituting cardiometabolic disorders and weight, which include central adiposity, elevated triglycerides, low levels of high-density lipoprotein, hypertension, and elevated blood glucose levels. The public health impact is clear when one considers that 38.9% of US adults report a prescription drug expense for a cardiovascular agent and 28.9% report similar expenses for metabolic agents. The latter are the number 1 type of medication prescribed in the United States. The P&T committee is uniquely positioned to provide knowledge and strategies to improve the treatment of patients with these conditions. (Formulary. 2009;44:276–279.)
The National Heart, Lung, and Blood Institute (NHLBI) estimates that almost 25% of US adults have a constellation of abnormalities constituting what was once called "syndrome X," and later, "metabolic syndrome" or "insulin resistance syndrome."1 The component disorders include central adiposity defined by waist circumference or hip-waist ratio, elevated triglycerides, low levels of high-density lipoprotein, hypertension, and elevated blood glucose levels.
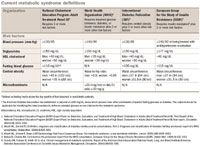
A further complication for healthcare professionals seeking to identify the most appropriate treatment strategies from current guidelines is that the American Diabetes Association (ADA) and the European Association for the Study of Diabetes do not recognize "metabolic syndrome" per se. Instead, they recommend that any patient with one cardiometabolic disorder be screened for the others and that each component disorder be treated to its individual target.8 In addition, current guidelines from the NHLBI-sponsored Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure (JNC 7) recommend a lower blood pressure goal for patients with diabetes than does ATP III,9 and current ADA treatment guidelines recommend earlier drug treatment-at the prediabetes level-especially for patients with other risk factors for developing type 2 diabetes, including hypertension, low HDL, elevated triglycerides, and obesity.10
Not only do the various treatment parameters conflict, they are updated often. For example, the NHLBI has convened experts to update both ATP and JNC guidelines, and the proposed new versions are expected to be available for public comment in December 2009. The ADA released its updated clinical practice guidelines earlier this year.10
The IDF emphasizes central obesity, defining a diagnosis when a person has obesity plus any two other risk factors.5 The World Health Organization focuses on glucose intolerance/resistance plus two other factors.6
ATP III further categorizes metabolic syndrome into major risk factors-smoking, hypertension, reduced HDL and elevated LDL cholesterol, family history of premature coronary heart disease, and aging-and into underlying risk factors, such as obesity, physical activity, and poor diet; and emerging factors, including elevated triglycerides, glucose intolerance, and insulin resistance.
Although many experts warn that diabetes is one of the major results of metabolic syndrome, WHO doesn't even consider elevated fasting glucose a risk. However, WHO does factor in microalbuminuria-another indication of the variability of the guidelines.
CLINICAL PHARMACY IMPLICATIONS
The P&T committee is the ideal group to coordinate a cross-therapeutic approach to addressing cardiometabolic disorders and weight. Thanks to its focus and expertise, the P&T committee is uniquely positioned to provide knowledge and practical strategies to improve the treatment of patients with metabolic conditions in the health system.
The fact that cardiovascular and metabolic agents are the two top-selling types of prescription drugs in the United States further highlights the importance of pharmacists and formulary decision-makers in the management of cardiometabolic health disorders-in both the health system and the community. One group of pharmacists cannot operate without being cognizant of the efforts of the other.
Patients depend on pharmacists working in community and health-system settings for advice and guidance, not only on medication usage, but also on lifestyle modification and the use of self-monitoring and testing devices. In the managed care arena in particular, streamlined disease management and enhanced care coordination for dyslipidemia, hypertension, diabetes, and obesity can greatly improve outcomes.
In the inpatient setting, providers depend on the P&T committee to offer data and insight into what medications will maintain and augment the efforts made by the patient and his or her health practitioners in the community. Such continuity of care can improve outcomes for the patient while he or she is being treated in the hospital or health system and after discharge.
PHARMACISTS' ROLE
As with many drugs, adherence is a growing problem, and those medications that are associated with the cardiometabolic disorders and weight-antihypertensives, obesity, and diabetes drugs-are no exception. Nonadherence occurs in 21.3% of patients with diabetes, according to a retrospective cohort study of 11,532 patients.11 The study revealed that those who did not adhere to their prescribed antihypertensive, hypoglycemic, and lipid-lowering medications at least 80% of the time were significantly more likely to have elevated levels of HbA1c, blood pressure, and LDL than those who adhered.
The American Pharmacists Association recommends that pharmacists collaborate with physicians to identify people who are not adherent and help eliminate barriers by minimizing the number of daily doses, reducing dosing frequency, and selecting the most efficacious and cost-effective medications.
Tracey H. Taveira, PharmD, associate professor of pharmacy at the University of Rhode Island in Kingston, says that pharmacists can play an important role in medication adherence as patients take more drugs as part of increasingly complex regimens. "We are [the] experts on the formulary, helping ensure that drugs are covered and converting doses and medications if needed," she says.
Through an affiliation with the Veterans Affairs Medical Center in Providence, Taveira and colleagues conducted a study of 375 veterans using the Cardiovascular Risk Reduction Clinic model.12 This was a pharmacist-coordinated care model incorporating cardiometabolic risk factors under one umbrella for treatment by clinical pharmacists overseen by a cardiologist. Participants underwent motivational interviewing to modify behavior and received frequent medication titrations, which clinical pharmacists were allowed to modify under federal regulation.
In accordance with guidelines recommended by the American College of Cardiology/AHA and the American Diabetes Association, 70.7% met the discharge criteria by the end of the study period. Guideline adherence increased for total cholesterol, LDL, HDL, HbA1c, and systolic blood pressure.
CLINICAL FOCUS: HYPERTENSION
The estimated direct and indirect cost of hypertension for 2009 is $73.4 billion.13 Among US adults, 29% have hypertension and 78% of them are aware of it. Diagnosed hypertension affects 51% of women and 45% of men aged 65 years and older, but when undiagnosed cases are considered, estimates of hypertension incidence are 78% for older women and 64% for older men.14 High blood pressure is particularly prevalent among US African Americans at 41.4%, and the incidence continues to increase.
Approximately 68% of patients with high blood pressure are taking antihypertensive medication, and of these, more than 64% are controlled. Despite this, hypertension-related deaths increased by 25.2% between 1995 and 2005, and the actual number of deaths increased by 56.4% during that time frame.15
"Prehypertension" is estimated to affect 25% of the adult population, and untreated systolic blood pressure of between 120 and 139 mm Hg is associated with increased risk for cardiovascular outcomes and events. In addition, patients with prehypertension are 1.65 times more likely than those with normal blood pressure to have elevated cholesterol levels, have diabetes, and be overweight or obese.15
CLINICAL FOCUS: LIPID DISORDERS
Despite increased awareness, less than half of patients qualifying for lipid-lowering therapy according to treatment goals for low-density lipoprotein (LDL) levels receive therapy-including those at the highest risk because they have symptomatic coronary heart disease. Further, only one-third of patients receiving lipid-lowering therapy are treated to target lipid levels and fewer than 20% of those with CHD are at goal levels.13
Low high-density lipoprotein (HDL) levels and elevated triglycerides are considered contributors to increased cardiovascular risk, independent of LDL levels. It is estimated that 15.5% of US adults have lower than optimal HDL cholesterol levels.
In addition, non-Hispanic white men and Mexican American men and women have estimated mean triglycerides above the recommended level.13
The prevalence of cardiometabolic disorders and weight and the subsequent costs can be addressed by a multidisciplinary approach stressing early detection and diagnosis, effective treatment, and patient education and compliance.
Disclosure Information: All authors and editors report no financial disclosures as related to products discussed in this article.
REFERENCES
1. National, Heart, Lung, and Blood Institute Diseases and Conditions Index. Metabolic syndrome. http://www.nhlbi.nih.gov/health/dci/Diseases/ms/ms_whoisatrisk.html. Accessed July 29, 2009.
2. National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III) final report. Circulation. 2002;106:3143–3421.
3. Soni A. Agency for Healthcare Research and Quality. Medical Expenditure Panel Survey. Statistical Brief #232. The top five therapeutic classes of outpatient prescription drugs ranked by total expense for adults age 18 and older in the US civilian noninstitutionalized population, 2006. http://www.meps.ahrq.gov/mepsweb/data_files/publications/st232/stat232.pdf. Accessed July 29, 2009.
4. Grundy SM, Cleeman JI, Merz CN, et al; National Heart, Lung, and Blood Institute; American College of Cardiology Foundation; American Heart Association. Implications of recent clinical trials for the National Cholesterol Education Program Adult Treatment Panel III guidelines.Circulation. 2004;110:227–239.
5. Alberti KG, Zimmet PZ. Definition, diagnosis and classification of diabetes mellitus and its complications. Part 1: Diagnosis and classification of diabetes mellitus provisional report of a WHO consultation. Diabet Med. 1998;15:539–553.
6. Alberti KG, Zimmet P, Shaw J; IDF Epidemiology Task Force Consensus Group. The metabolic syndrome–a new worldwide definition. Lancet. 2005;366:1059–1062.
7. Balkau B, Charles MA. Comment on the provisional report from the WHO consultation. European Group for the Study of Insulin Resistance (EGIR). Diabet Med. 1999;16:442–443.
8. Kahn R, Buse J, Ferrannini E, Stern M; American Diabetes Association; European Association for the Study of Diabetes. The metabolic syndrome: Time for a critical appraisal: Joint statement from the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2005;28:2289–2304.
9. Chobanian AV, Bakris GL, Black HR, et al; National Heart, Lung, and Blood Institute Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure; National High Blood Pressure Education Program Coordinating Committee. The Seventh Report of the Joint National Committee on the Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: The JNC 7 report. JAMA. 2003;289:2560–2572.
10. American Diabetes Association. Standards of medical care in diabetes–2009. Diabetes Care. 2009;32(suppl 1):S13–S61.
11. O'Connor PJ. Improving medication adherence: Challenges for physicians, payers, and policy makers. Arch Intern Med. 2006;166: 1802–1804.
12. Taveira TH, Wu WC, Martin OJ, Schleinitz MD, Friedmann P, Sharma SC. Pharmacist-led cardiac risk reduction model. Prev Cardiol. 2006;9:202–208.
13. Lloyd-Jones D, Adams R, Carnethon M, et al; American Heart Association Statistics Committee and Stroke Subcommittee. Heart disease and stroke statistics–2009 update: A report from the American Heart Association Statistics Committee and Stroke Statistics Subcommittee. Circulation. 2009;119:e21–e181.
14. Robinson K. Trends in health status and health care use among older women. Aging Trends, no. 7. Hyattsville, Md: National Center for Health Statistics; 2007.
15. Greenlund KJ, Croft JB, Mensah GA. Prevalence of heart disease and stroke risk factors in persons with prehypertension in the United States, 1999-2000. Arch Intern Med. 2004;164:2113–2118.
FDA Approves Combination Therapy for Pulmonary Arterial Hypertension
March 25th 2024J&J’s Opsynvi is single-tablet combination of macitentan, an endothelin receptor antagonist, and tadalafil, a PDE5 inhibitor. It will be priced on parity with Opsumit, which is also a J&J product to treat patients with PAH.
FDA Issues Complete Response Letter for Onpattro in Heart Failure Indication
October 9th 2023Alnylam Pharmaceuticals will no longer pursue this indication of Onpattro and will instead on focus on a label expansion for Amvuttra, which is in phase 3 development to treat patients with cardiomyopathy of ATTR amyloidosis.
